Federal Support for Graduate Medical Education: An Overview
Access to health care is, in part, determined by the availability of physicians, a function of the physician supply. Policymakers have demonstrated a long-standing interest in access to care, both in general and for specific populations. Moreover, federal support for medical residency training (a.k.a., graduate medical education [GME]) is the largest source of federal support for the health care workforce. Although the health workforce includes a number of professions, the size of the federal investment in GME—estimated at $16 billion in 2015—makes it a policy lever often considered to alter the health care workforce and impact health care access. This report describes federal programs that provide GME support. Although these programs may also support training for other health professions, this report focuses on training for physicians, who receive the bulk of GME support. The report examines GME support in Medicare, Medicaid, the Department of Veterans Affairs, the Department of Defense, and programs administered by the Health Resources and Services Administration, such as the Children’s Hospital and Teaching Health Center GME payment programs. The report details the mechanisms that various federal programs use to support GME and provides data, when available, on funding and the number of trainees. As noted in the table below, the data available vary by program. Program Name Control over trainees Total Funding Number of Trainees Cost Per Trainee
MANDATORY FUNDING
Medicare GME Payments The number of Medicare-supported residents and per-resident payment amount is capped for each hospital, but hospitals determine staffing needs and types of residents with the exception of certain primary care residents. FY2015 (est.): $10.3 - $12.5 billion
FY2015 (est.): 85,712 - 87,980 FTE (DGME) slots 85,578 - 88,416 FTE (IME) slots FY2015 (est. average): $112,000 - 129,000 per FTE
Medicaid GME Payment States are permitted to make these payments using their own criteria to determine which providers are eligible for payments. N/A. N/A The Medicaid program does not require states to report these data. N/A. The Medicaid program does not require states to report these data.
Teaching Health Centers GME Payment Program Funding to applicant teaching health centers that meet the program’s eligibility requirements. FY2018: $126.5 million (est.)
AY2016-AY2017: 742 FTE slots 771 total residents trained N/A.
DISCRETIONARY FUNDING
Veterans Affairs GME Payments VA facilities determine their staffing needs and the number and type of residents supported. FY2017: $1.78 billion AY2016-AY2017: 11,000 FTE slots and
43,565 residents spent part of their training at a VA facility FY2015 (est.): $137,792/resident
Children’s Hospital GME Payment Program Grant funding awarded to applicant children’s hospitals that meet the program’s eligibility requirements. FY2019: $325 million FY2016-FY2017 58 hospitals received payments to support 7,164 FTE slots N/A
Department of Defense GME Payments Divisions of the armed forces determine their staffing needs and the number and type of residents supported. FY2012: $16.5 million FY2017: 3,983 FTE residents N/A
Sources: CRS analysis of agency data, including review of various agency budget justification and The Robert Graham Center program data sourced from CMS Medicare hospital cost report data, and GAO report, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding (GAO-18-240, 2018). Notes: AY = Academic year; Academic year 2016-2017 began on July 1, 2016, and concluded on June 30, 2017. DGME = direct graduate medical education. est. = estimate. FTE = full time equivalent. FY = fiscal year. IME = Indirect Medical Education. N/A = not available. VA = the Department of Veterans Affairs.
Federal Support for Graduate Medical Education: An Overview
Jump to Main Text of Report
Contents
- Federal Role in GME
- GME Policy and Health Workforce Data
- Federal GME Support
- Medicare
- The Medicare GME Cap
- Medicare DGME Payments
- Medicare IME Payments
- Medicaid
- Department of Veterans Affairs (VA)
- Health Resources and Services Administration
- Children's Hospitals GME
- Teaching Health Center GME
- Department of Defense (DOD)
- Concluding Observations
Figures
Tables
Summary
Access to health care is, in part, determined by the availability of physicians, a function of the physician supply. Policymakers have demonstrated a long-standing interest in access to care, both in general and for specific populations. Moreover, federal support for medical residency training (a.k.a., graduate medical education [GME]) is the largest source of federal support for the health care workforce. Although the health workforce includes a number of professions, the size of the federal investment in GME—estimated at $16 billion in 2015—makes it a policy lever often considered to alter the health care workforce and impact health care access. This report describes federal programs that provide GME support. Although these programs may also support training for other health professions, this report focuses on training for physicians, who receive the bulk of GME support. The report examines GME support in Medicare, Medicaid, the Department of Veterans Affairs, the Department of Defense, and programs administered by the Health Resources and Services Administration, such as the Children's Hospital and Teaching Health Center GME payment programs. The report details the mechanisms that various federal programs use to support GME and provides data, when available, on funding and the number of trainees. As noted in the table below, the data available vary by program.
|
Program Name Control over trainees |
Total Funding |
Number of Trainees |
Cost Per Trainee |
|
MANDATORY FUNDING |
|||
|
Medicare GME Payments The number of Medicare-supported residents and per-resident payment amount is capped for each hospital, but hospitals determine staffing needs and types of residents with the exception of certain primary care residents. |
FY2015 (est.): |
FY2015 (est.): |
FY2015 (est. average): |
|
Medicaid GME Payment States are permitted to make these payments using their own criteria to determine which providers are eligible for payments. |
N/A. |
N/A The Medicaid program does not require states to report these data. |
N/A. The Medicaid program does not require states to report these data. |
|
Teaching Health Centers GME Payment Program Funding to applicant teaching health centers that meet the program's eligibility requirements. |
FY2018: |
AY2016-AY2017: |
N/A. |
|
DISCRETIONARY FUNDING |
|||
|
Veterans Affairs GME Payments VA facilities determine their staffing needs and the number and type of residents supported. |
FY2017: |
AY2016-AY2017: |
FY2015 (est.): |
|
Children's Hospital GME Payment Program Grant funding awarded to applicant children's hospitals that meet the program's eligibility requirements. |
FY2019: |
FY2016-FY2017 |
N/A |
|
Department of Defense GME Payments Divisions of the armed forces determine their staffing needs and the number and type of residents supported. |
FY2012: |
FY2017: |
N/A |
Sources: CRS analysis of agency data, including review of various agency budget justification and The Robert Graham Center program data sourced from CMS Medicare hospital cost report data, and GAO report, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding (GAO-18-240, 2018).
Notes: AY = Academic year; Academic year 2016-2017 began on July 1, 2016, and concluded on June 30, 2017. DGME = direct graduate medical education. est. = estimate. FTE = full time equivalent. FY = fiscal year. IME = Indirect Medical Education. N/A = not available. VA = the Department of Veterans Affairs.
Access to health care is, in part, determined by the supply of physicians available to provide treatment. Physician supply is a function of the number of physicians trained, how long they remain in practice, their productivity, and the hours they work. Policymakers have demonstrated a long-standing interest in access to care (in general and for specific populations). The federal government has identified certain health workforce concerns and creates programs that seek to address these concerns. Specifically, the Government Accountability Office (GAO) estimated that the Department of Health and Human Services (HHS) administers 72 health workforce programs.1 Among these programs are those that seek to increase access to physician services, including programs that encourage people to enter primary care to address identified concerns that there are too few primary care physicians relative to the number of physician specialists.2
Federal programs also exist to recruit and retain physicians in rural areas because of concerns that the populations that reside in these areas lack access to care. Specifically, the federal government designates some areas as medically underserved or as health professional shortage areas (HPSA) and provides benefits (e.g., higher Medicare payment rates) to providers who practice in these areas.3 In addition to these programs and policies, the federal government provides support for medical residency training (a.k.a., graduate medical education [GME]). Specifically, through payments that are generally made to hospitals, the federal government pays some of the costs that hospitals and other health providers incur when training residents. Such costs include, but are not limited to residents' and supervisors' salaries, and the costs of extra medical tests that residents may order as part of their training.
The federal government makes a significant investment in GME—according to GAO, GME programs account for nearly three-quarters of HHS's health workforce expenditures4—and GME may be a strong policy lever to impact access because the number of medical school graduates who obtain and complete a residency determines the size of the physician workforce, and the types of residencies they complete determine its specialty composition. Finally, where physicians complete their residencies often affects where they establish their practices.5 Given the influence of residency training on the physician population, policies that alter federal funding for GME may affect future physician supply and could be used to address identified workforce concerns.
This report provides an overview of federal GME support; it discusses whether a particular source of federal GME support is actively used to further workforce goals such as altering the geographic or specialty distribution of residents trained. A number of GME critiques have raised concerns about the data that the federal government collects on these programs; for example, whether the data available are sufficient to determine program effectiveness.6 This report details programmatic data gaps where they have been identified. It does not summarize recent GME critiques in detail; for readers interested in such critiques, Appendix A provides some sources for further reading.
Some federal programs use GME to support training for non-physician health providers; however, this report focuses only on the training of physicians.7 To be licensed to practice independently in a state, physicians in the United States must complete a minimum of three years of GME, with additional years required depending on their specialty.8 In Academic Year (AY) 2016-2017, approximately 124,000 individual residents were in training,9 including approximately 21,000 fellows10—medical school graduates who have completed their initial residency training and are continuing their training in a fellowship in a subspecialty.11 (See text box for definitions.) GME generally takes place in hospitals that sponsor residency programs in specific specialties (e.g., pediatrics or surgery). Hospitals choose the number and specialties of the residents they train, but must meet accrediting body standards that attempt to assure that hospitals have the facilities, staffing, and patient load necessary to ensure that residents will receive adequate training in their chosen specialty (see text box). During their residency, residents rotate to outpatient facilities or other hospitals to gain experience treating different populations in different settings. Specific residency training requirements vary by specialty and are determined by the accrediting bodies.12
|
Selected GME Definitions Medical Resident: An individual who has completed medical school and is in training to become a licensed physician. Residents generally train in a specialty for three to five years (although some specialties require a preliminary year of general medical training before specialty training commences). Obtaining a medical residency is competitive; medical students in their final year apply to residency programs in a particular location and specialty. Medical residents are paid a salary during residency, but this salary is generally a fraction of what they will earn after completing their residency. Primary Care Residents: Generally refers to physicians who are in training in family medicine, internal medicine, and pediatrics. Other definitions may also include geriatrics and obstetrics and gynecology. Specialty Residents: Physicians who are in training in, a medical specialty that is not considered primary care (e.g., anesthesiology). Fellows: Physicians who have completed an initial residency in primary care or a specialty and are pursuing additional specialty training. For example, an internal medicine resident who pursues additional training in cardiology would be considered to be a cardiology fellow. Initial Residency Period (IRP): The minimum number of years required for a resident to become board-eligible in the specialty in which the resident first begins training. The IRP for a specialty is based on the minimum accredited length of a residency program, as determined by the Accreditation Council for Graduate Medical Education (ACGME) and the American Osteopathic Association (AOA) (see also entry for "Accredited Program"). Board-Eligible: A physician who has completed the requirements for admission to a medical specialty board, but has not passed the required board examination. For example, a resident must complete three-years of training in an internal medicine residency program to be eligible for certification by the American Board of Internal Medicine. Teaching Hospital: A hospital that offers one or more accredited residency (or fellowship) programs; and is therefore, eligible to receive GME payments from federal programs. Teaching hospitals are often affiliated with a medical school. Accredited Program: A residency or fellowship program that meets certain standards set by the accrediting body (ACGME or the AOA). The two systems are merging to create a single accreditation system that should be fully in effect in 2020. Academic Year (AY): The year beginning July 1when residents either begin their training or move up to the next year within their training. For example, AY2018-AY2019 began on July 1, 2018 and will end on June 30, 2019. Sources: Association of American Medical Colleges, "The Road to Becoming a Doctor," https://www.aamc.org/download/68806/data/road-doctor.pdf; Association of American Medical Colleges, "Medicare Payments for Graduate Medical Education: What Every Medical Student, Resident, and Advisor Needs to Know," https://members.aamc.org/eweb/upload/Medicare%20Payments%20for%20Graduate%20Medical%20Education%202013.pdf; American Association of Colleges of Osteopathic Medicine, "Single Accreditation System," http://www.aacom.org/news-and-events/single-gme; Medicare Payment Advisory Commission's June 2009 Report to Congress: Improving Incentives in the Medicare Program, Chapter 1, at http://www.medpac.gov/documents/reports/Jun09_Ch01.pdf?sfvrsn=0; and 42 U.S.C. 293l=1(f)(2). |
Federal Role in GME
The federal government makes significant investments in GME funding through various programs.13 In FY2012, the last year of data available for all federal sources of GME payments, the federal government spent an estimated $15 billion on GME, which was the largest federal investment in the health care workforce.14 More recent data analyzed by GAO found that GME programs administered by the Department of Health and Human Services (HHS) and the Department of Veterans Affairs (VA) spent $14.5 billion on GME in 2015, but their work did not analyze Department of Defense GME spending. As such, 2012 remains the most recent year of a total federal GME estimate. Using their 2012 estimate, GAO found that 78% of government-wide health workforce funding was for GME; with Medicare payments accounting for 85% of this funding.15 Similarly, a GAO analysis of HHS programs in FY2014, found that HHS supported 72 health workforce programs, but that nearly three-quarters of all spending was from Medicare GME payments.16
The federal government supports GME
- through payments made by the Medicare and Medicaid programs, both administered by the Centers for Medicare & Medicaid Services (CMS) located in HHS;
- by training medical residents at Department of Veterans Affairs (VA) and Department of Defense (DOD) facilities;
- and by funding programs administered by HHS's Health Resources and Services Administration (HRSA) that support primary care training in outpatient facilities, rural GME program development, and training in children's hospitals.
The federal government's primary role in GME has been as a payer. In this role, it has a significant influence on the physician workforce, but this role has generally been passive, because, with some exceptions, the federal government has little involvement through its support of GME in the content of training, the specialties it pays for, or training locations.17 In addition, the government's role in GME has generally not been linked to other federal health workforce investments, such as investments made to train non-physician providers whose work could complement or, where appropriate, replace that of physicians and who could be trained at a lower cost.18
These critiques have been raised particularly with regard to Medicare's GME support because it is the largest source of federal GME support, estimates of Medicare GME payments range from approximately $10.3 to $12.5 billion in FY2015.19 Medicare is also frequently discussed because, unlike other sources of GME support, it explicitly limits (i.e., caps) the number of residents it supports.20 Some argue that this limit makes increasing the number of residents and changing the locations where they train difficult. This argument generally does not take into account GME growth that occurred despite the Medicare cap. For example, recent work by GAO found that the number of residents in training grew by 22% over the 10-year period they examined (2005 to 2015), although the geographic areas where residents trained remained largely unchanged.21 Another analysis estimates that the number of residents in training grew by 27% during the 20-year period since the Medicare limit on GME support was enacted.22 This may be the case because the Medicare cap is not an absolute, and other sources—for example, other federal programs, state and local government funds, or hospital funds—can be used to expand or alter the number and types of residents in training. In addition, new hospitals can begin training residents and receive Medicare payment for doing so.23
Some argue that Medicare's residency limit should be partially or fully removed to address physician shortages in certain geographic areas and medical specialties.24 And Members of Congress have introduced legislation that would do so.25 Others argue that expanding Medicare support, unless done in a way that is directive; for example, by explicitly allocating positions to hospitals in specific geographic areas or requiring hospitals to fund residency positions in certain specialties, would not address identified workforce issues such as too few physicians in certain areas or practicing primary care.26 GAO also found that although there are incentives within Medicare and other programs to increase training in rural areas, hospitals frequently did not take advantage of them.27
GME Policy and Health Workforce Data
The federal government supports workforce data collection and projections of future needs; in addition, researchers and advocates also collect and disseminate such data.28 Such data are necessary inputs for GME policy but are not sufficient. Determining the appropriate GME policy is inherently challenging because training a new physician is a long process; as such, attempting to change the physician workforce through changes to GME requires a long time horizon and good initial data to project the future need for physicians. This process of projection is particularly challenging because policy changes may occur in the interim that alter the assumptions used in the projections.
Recent projections conducted by the National Center for Health Workforce Analysis, at HRSA, demonstrate the challenges of making projections concurrent with policy changes. In their 2013 projections, they projected that there would be a primary care physician shortage in 2020, but that the magnitude could vary greatly depending on assumptions about the role of non-physician providers. Specifically, they projected that the number of primary care physicians would grow by 8% between 2010 and 2020, but that the demand for their services would grow by 14%.29 They based this on the demand for services at the time of the study and assumptions about the future aging of the population, and the expected increase in insurance coverage driven by the Patient Protection and Affordable Care Act (ACA, P.L. 111-148, as amended). These projections do not reflect more recent policy changes and stakeholder responses to the implementation of the ACA that may have affected insurance coverage and related demand for health services. The projections assumed that all states would expand Medicaid under the ACA, that full Medicaid expansion has not occurred,30 and that these projections also do not account for changes in federal policy related to the private insurance market. For example, beginning in 2019 individuals will no longer have to maintain insurance coverage or pay a penalty (i.e., the ACA's individual mandate), which experts predict will reduce insurance coverage.31 These policy changes may mean that HRSA's projected 2020 shortages may not occur or may be less than were estimated in 2013.
Another source of uncertainty in physician projections is the size and role of non-physician providers. Specifically, the HRSA model that predicted the most extreme shortages projected that there would be a shortage of 20,400 primary care physicians in 2020, while other HRSA models that include full use of nurse practitioners and physician assistants project that the shortage would be 6,400.32 Estimates commissioned by the American Association of Medical Colleges (AAMC)—a private, nonprofit organization that represents U.S.-accredited medical schools and some teaching hospitals—vary depending on assumptions made about the ability of nurse practitioners and physician assistants to augment physician supply. Specifically, in projections to 2030, the shortage of primary care physicians ranged between 7,300 and 43,100.33 Others have suggested that increasing the role of these providers and the use of new care models may be sufficient to avert shortages.34
Experts also project geographic shortages both overall and of specific provider types and specialties. As noted, some areas are currently designated as being in shortage.35 GAO also found that there has been little change in the areas where GME training occurs, which may affect where physicians ultimately practice.36 As with general estimates of physician supply, the role of nurse practitioners and physician assistants may alter predicted geographic area shortages. It is also possible that targeted policy changes either already enacted or if enacted at the federal or state levels could alleviate geographic shortages in the areas they target.37
The uncertainty inherent in projecting supply and demand under changing policy conditions demonstrates the need to regularly update these projections to incorporate the latest data and policy conditions. The general uncertainty about the future need for physicians makes it challenging to develop and implement GME policy. 38 However, it is relatively clear that good data are needed both to examine the overall health workforce and to determine how GME investments can be better aligned to achieve overall health workforce goals. The need for improved data collection has also been recommended in several of GAO's recent reports that examine GME spending.39
Federal GME Support
The federal government supports the health workforce generally, and the physician workforce specifically, through a number of programs, including those that provide loan repayment or scholarships to physicians.40 More than three-quarters of federal workforce support is through GME.41 The programs below are organized by relative size, as determined by the amount that the program spends annually. These programs are also briefly summarized in Appendix B.
Medicare
Medicare is by far the largest source of GME support.42 Medicare began supporting GME when the program was enacted in 1965. Congress stated that educational activities enhance the quality of care at a medical institution and therefore education costs should be borne by Medicare to an appropriate extent.43
Medicare provides funding for GME, paying "its share" of costs. Medicare provides GME payments based on a number of factors, including a teaching hospital's full-time equivalent (FTE) residents. However, Medicare GME funding is not tied to a specific resident. Instead, multiple residents may occupy one FTE because not all time is counted for Medicare purposes (e.g., time spent at facilities operated by the VA would not be paid by Medicare). In FY2015, estimates of what Medicare provided in overall GME payments range from approximately $10.3 to $12.5 billion.44 Medicare GME payments are made under two distinct methods: direct graduate medical education payments (DGME) and indirect medical education payments (IME). Under these two payment methods, the number of FTE residents that a hospital may receive payment for is limited, or "capped."
|
Different Estimates of Medicare GME Payments and FTEs CMS does not publish estimates of Medicare GME payments and the FTEs supported by such payments. The estimates presented in this report are from non-CMS sources, including CRS. Estimates included in this report are calculated using CMS-published cost report data. However, the estimates in this report differ by source. And the differences are due to both known and unknown variations in the purpose and methodology used to calculate these estimates. For example, some of the difference between the GAO and CRS estimates is due to the kinds of hospitals included in the analysis (e.g., CRS excluded Inpatient Psychiatric Facilities (IPFs) and Inpatient Rehabilitation Facilities (IRFs), GAO included these types of hospitals). However, even when accounting for known methodological decisions, estimates still differed. CRS was unable to determine all of the reasons for the differences in estimates. The ranges contained in this report are based on three estimates of FY2015 Medicare GME payments and FTEs One estimate is calculated and published by GAO using CMS data (see GAO-18-240, 2018, https://www.gao.gov/assets/700/690581.pdf). A second estimate is based on CRS calculation of GME data published by the Robert Graham Center, a policy research center that provides analysis for physicians and the American Academy of Family Physicians. The Graham Center publishes Medicare GME payment and FTE data tables by hospital for each fiscal year; this data are sourced from CMS's Medicare cost report data.45 The third estimate is calculated by CRS using CMS-published hospital cost report data. Table 1 contains the three dollar and FTE estimates, and Table B-1 in Appendix B contains the ranges based on these three sources' estimates. |
CMS has not traditionally considered its role to be one of directing the physician workforce.46 Specifically, except for some statutory requirements related to the use of certain "redistributed" GME slots for primary care and for sparsely populated geographic areas, CMS generally does not direct hospitals to train certain types of residents, nor does it require training be in specific geographic areas, or dictate the content of training programs.47 Rather, CMS collects some GME related information from hospitals and uses it for payment calculation and auditing to ensure hospitals are paid according to GME statutes and regulations. CMS does not use this information to evaluate its GME investment or to otherwise direct the composition of the physician workforce.48
The Medicare GME Cap
Medicare's GME support was initially open-ended, where Medicare would pay for additional FTE residents that hospitals trained. In 1997, graduate medical education stakeholders released a consensus statement arguing that the United States was on the verge of a serious oversupply of physicians and recommending limiting federal funding of GME positions to more align with the number of graduates of accredited U.S. medical schools.49 Congress enacted the Balanced Budget Act of 1997, (P.L. 105-33), which limits Medicare's GME—most hospitals would receive DGME and IME support only for the number of allopathic and osteopathic FTE residents it had in training in 1996; in other words, each hospital was given a limit in terms of the number of positions or slots that Medicare would fund.50
Slots may be occupied by residents or fellows. Slots do not directly correspond to a specific resident or fellow because residents or fellows may spend periods of a given year at different facilities, or doing research. During these times, residents are not counted by the sponsoring hospital. Residents may not be counted simultaneously for payment by two government programs.51
This "cap" on the number of FTE residents Medicare will support is calculated for each hospital.52 However, the cap is not absolute—Medicare provides GME funding to new hospitals that previously did not have residency programs—either newly constructed hospitals or existing hospitals that develop new training programs—and the GME cap is not calculated and implemented until the new teaching programs' fifth year.53 Since the Medicare cap was enacted, hospitals have expanded the number of residents they are training by using non-Medicare sources of support (such as, hospital revenue or state and local funds).54 Specifically, in the 20 years since the cap was enacted, the number of residency slots has increased by 27%. Generally, these increases have been in subspecialties (i.e., for fellowship training); subspecialty services tend to generate higher revenue or impose lower cost burden on hospitals.55 In addition, Medicare GME slots have been redistributed since the cap was enacted; for example, the ACA included two redistribution programs—the first redistributed unused slots, and the second continually redistributes slots from closed hospitals.56
|
Medicare GME Payments |
Medicare GME FTEsa |
||||
|
Source |
DGME |
IME |
Total |
DGME |
IME |
|
CRS |
$3,682,896,679 |
$7,380,498,587 |
$11,063,395,226 |
85,712 |
85,578 |
|
GAO |
$3,709,961,953 |
$6,624,556,072 |
$10,334,518,025 |
87,980 |
88,416 |
|
Graham Center |
$3,722,246,061 |
$8,738,082,792 |
$12,460,328,853 |
111,160 |
|
Sources: CRS analysis of FY2015 Medicare hospital cost report data as reported to the CMS Healthcare Cost Report Information System; figures published by GAO, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding (GAO-18-240, 2018), https://www.gao.gov/assets/700/690581.pdf; and CRS calculation using Medicare GME data published by The Robert Graham Center, https://www.graham-center.org/rgc/maps-data-tools/data-tables/gme.html. The Graham Center's website states that the GME data table they publish is sourced from CMS cost report data.
Notes: The differences in dollar and FTE estimates between the three sources in this table are due to both known and unknown variations in the purpose and methodology used to calculate these estimates. For additional information, see "Different Estimates of Medicare GME Payments and FTEs" in the "Medicare" section of this report.
FTEs = Full-Time Equivalents; GME = Graduate Medical Education; DGME = Direct Graduate Medical Education; IME = Indirect Medical Education; CRS = Congressional Research Service; GAO = Government Accountability Office.
a. DGME and IME FTEs are not unduplicated, therefore, a total is not included.
Medicare DGME Payments
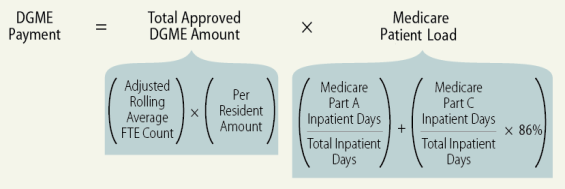
In FY2015, Medicare provided $3.68 billion in DGME payments to teaching hospitals, supporting approximately 85,700 FTE residents.57 Medicare DGME payments reimburse teaching hospitals for the Medicare portion of approved program costs directly incurred with residency programs, such as resident stipends, supervisory physician salaries, and administrative costs. However, Medicare does not reimburse the teaching hospital for the actual costs incurred by the residency program, but is instead the product of the total approved DGME costs and the hospital's Medicare patient load percentage (see Figure 1).58 Under this methodology, Medicare pays for its share of the approved program costs associated with the residency program, whereas non-Medicare payers (e.g., a private insurer) would theoretically cover the remaining costs of the residency program based on their patient share at the teaching hospital.
In general, the total approved DGME cost is based on a teaching hospital's approved weighted FTE count, subject to a cap, and a prospectively determined per-resident amount. Residents in their initial residency period (IRP) are weighted as 1.0 for the FTE count, whereas residents past their IRP are weighted as 0.5 for the FTE count. The hospital's approved FTE count is a rolling average of the hospital's FTE count over the past three years. The per-resident amount is a dollar value based on the amount of costs of the hospital's residency program for each FTE resident in a base period (a hospital's cost reporting period beginning on or after October 1, 1983, but before October 1, 1984) and is updated each year.59 The product of these two figures represents Medicare's total approved DGME amount for a teaching hospital in a given year. The Medicare patient load is based on the teaching hospital's number of Medicare Part A inpatient days out of the total inpatient days plus 86% of Medicare Part C (Medicare Advantage) inpatient days out of the total inpatient days.60
 |
|
Sources: CRS analysis of Title XVIII of the Social Security Act (SSA) and relevant regulations. Note: The adjusted rolling average FTE count is subject to the GME cap. |
Medicare IME Payments
In FY2015, Medicare provided $7.38 billion in IME payments to teaching hospitals, supporting approximately 85,600 FTE residents.61 Medicare IME payments support the indirect costs associated with residency programs, such as the higher patient care costs from additional testing that residents may order as part of their training.62 Because Medicare's inpatient payment method, the Inpatient Prospective Payment System (IPPS), does not typically provide separate payment for additional testing, teaching hospitals may be disadvantaged by training residents under this payment method. To adjust for this possibility, Medicare IME payments are provided as a percentage increase to Medicare's IPPS payment (a sum payment amount of separate operating and capital components) for each discharge based on a statutory payment formula.
Medicare's formula for IME payment adjustment to the operating component of the IPPS payment is explicitly constructed in statute and is based primarily on an intern and resident-to-bed (IRB) ratio (see Figure 2).63 The IME operating adjustment is the percentage increase to Medicare's IPPS operating per-discharge payment.
IPPS payments also include a relatively smaller component that reflects the capital costs of the hospital.64 CMS constructed the IME capital adjustment formula and uses a residents-to-average daily census ratio (RADC) (not to exceed 1.5) to increase the teaching hospital's capital payment component under the IPPS (see Figure 2). Residents are counted in the same manner as in the IME operating adjustment formula. The addition of the IME percentage increases to Medicare IPPS operating and capital per-discharge payments amounts reflects Medicare's IME payments.
Medicaid
Medicaid provides the second-largest source of GME support.65 Medicaid is a joint federal-state program. States must follow broad federal rules to receive federal matching funds, but they have flexibility to design their own versions of Medicaid within the federal statute's basic framework. The federal statute does not require states to make Medicaid GME payments, but states are allowed to make Medicaid GME payments, and most states have historically made these payments.66
Unlike for Medicare or other federal GME payment systems, there is no federal guidance for Medicaid GME, so, states have significant flexibility in designing and administering their Medicaid GME payments.67 As a result, states' Medicaid GME payments vary substantially. States make Medicaid GME payments through the fee-for-service (FFS) delivery system, managed care delivery system, or both systems.68
Data for Medicaid GME payments are limited. CMS began collecting information about Medicaid GME payments made through the FFS delivery system in FY2010 through the CMS-64 data.69 Other information about Medicaid GME payments is available from the AAMC and GAO. AAMC conducts a 50-state survey about Medicaid GME payments every two to three years.70 GAO recently released a report on federal sources of GME payments that includes a survey of states regarding Medicaid GME payments.71 The information from these three sources varies and each source has limitations.
Table 2 shows the information about Medicaid GME payments from the three sources for a similar timeframe (i.e., federal fiscal year 2015 and state fiscal year 2015).72 The CMS-64 data reported only FFS GME payments, while the AAMC and GAO data included total GME payments including both FFS and managed care payments.73
|
Source |
Number of States with Medicaid GME Payments |
Amount of Medicaid GME Payments |
||||
|
FFS |
Managed Care |
Total |
FFS |
Managed Care |
Total |
|
|
CMS-64 Data (FY2015) a |
31 states |
NA |
31 states |
$1.6 billion |
NA |
NA |
|
AAMC Medicaid Survey |
41 states |
26 states |
43 states |
NA |
NA |
$4.3 billion |
|
GAO GME Report |
44 states |
20 states |
45 states |
NA |
NA |
$4.2 billion |
Sources: Congressional Research Service (CRS) analysis of Centers for Medicare & Medicaid Services, FY2015 CMS-64 data, as of December 1, 2016; Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, Association of American Medical Colleges, 2016; and U.S. Government Accountability Office, Physician Workforce HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding, GAO-18-240, March 2018.
Notes: The District of Columbia is counted as a state. The amounts of GME payments are total funds, which include both the federal and state share of the Medicaid GME payments.
AAMC = Association of American Medical Colleges; FFS = Fee-for-service; FY = Fiscal year; GAO = Government Accountability Office; NA = Not available; SFY = State fiscal year.
a. For the CMS-64 data, the Medicaid GME payments made through managed care are not disaggregated from the total managed care expenditures.
b. Six states have AAMC-estimated payment amounts or reported data from a different state fiscal year. Also, six states were unable to report Medicaid GME payments made through FFS versus payments made through managed care, but were able to report a total Medicaid GME payment amount
c. Seventeen states were either (1) unable to report exact payment amounts and only provided estimates or (2) unable to report any estimate of Medicaid GME payments. States reported the GME data for different timeframes with 39 states reporting data for SFY2015, four states reporting data for the 2015 calendar year, and two states reporting data for FY2015.
With respect to the number of states with Medicaid GME payments, Table 2 shows the AAMC and GAO surveys reported a similar number of states making Medicaid GME payments, with AAMC reporting 43 states for SFY2015 and GAO reporting 45 states for FY2015.74 The CMS-64 data differed from the AAMC and GAO data because it showed only 31 states with Medicaid GME payments. The CMS-64 data only included information about FFS GME payments, but the AAMC and GAO data reported 41 and 44 states, respectively, with FFS GME payments.75
The Medicaid GME payments (including both the FFS and managed care payments) from the AAMC and GAO surveys were similar, with AAMC reporting $4.3 billion in Medicaid GME payments for SFY2015 and GAO reporting $4.2 billion for SFY2015.76
The $1.6 billion in FFS Medicaid GME payments reported in the CMS-64 data for FY2015 is somewhat higher than the $1.4 billion in FFS Medicaid GME payments reported in the AAMC survey for SFY2015. However, the CMS-64 reports 31 states, and the AAMC data reports 41 states with FFS GME payments.77
AAMC and GAO provided additional information about Medicaid GME payments that is not included in the CMS-64 data. For instance, both sources have information about how the Medicaid GME payments were calculated. Some states used the Medicare methodology or a similar method, while other states used a per-resident payment based on the teaching site's share of total Medicaid revenues, costs, or patient volume.78 A few states paid a fixed amount per Medicaid discharge.79
AAMC and GAO reported information about the types of professions eligible for Medicaid GME payments. Most states supported training programs for physician residents, and some states supported training programs for other health professions, such as nurse practitioners, nurses, physician assistants, dentists, podiatrists, and allied health professionals.80
GAO collected information about the activities states intended the Medicaid GME payments to support, which include the salaries and benefits of residents and/or faculty, costs of administering the training program, and indirect medical education costs.81
Department of Veterans Affairs (VA)
Training health care professionals—including physicians—is part of the VA's statutory mission. It does so to provide an adequate supply of health professionals overall and for the VA's health system.82 In general, each year approximately 43,000 individual physician residents receive their clinical training by rotating through about 11,000 VA-funded physician FTE residency positions at VA medical facilities.83 In FY2017, the VA spent approximately $1.78 billion for GME, which was 80% of all VA stipend support for clinical training programs.84 The VA estimates it spent $0.89 billion in direct GME costs and the same amount ($0.89 billion) on indirect medical costs and an estimated $138,000 per FTE resident, which was higher than Medicare (and other programs) amount spent per resident. 85
Generally, the VA does not operate its own GME programs because accrediting bodies require that medical residents see a diverse population in terms of age, sex, and medical conditions throughout their training, which the VA's patient population generally does not provide. Instead, the VA partners with teaching hospitals, and residents from those hospitals' training programs rotate to a VA medical facility for a period of time.86 About 99% of VA's GME programs are sponsored by academic affiliates.87 The VA estimates that it partners with over 2,000 ACGME accredited programs in 80 different specialties or subspecialties.88 When the VA partners with a teaching hospital that operates a residency program, it shares the costs of faculty and residents when the residents are training at the VA medical facility. During the time that residents are at a VA facility, they are not counted for the purposes of the Medicare GME cap (and are not paid using Medicare funds). This permits hospitals to train additional residents above their Medicare FTE cap to account for the time that residents are at VA facilities and therefore being paid by the VA.
Unlike Medicare and Medicaid, the VA does control the type of residents it trains and where these residents are located. Each VA medical facility may determine its staffing needs and the types of programs it partners with academic affiliates to operate.89 As a result, the VA has data on the residents it trains and makes attempts to track whether its physician employees spent part of their residency training at the VA.90
The Veterans Access, Choice, and Accountability Act of 2014 (P.L. 113-46, as amended), among other things, included a requirement for the VA to expand the number of residents it trains by up to 1,500 positions in primary care, mental health, and other high-priority areas for the VA over a period of five years; however, subsequently the Jeff Miller and Richard Blumenthal Veterans Health Care and Benefits Improvement Act of 2016 (P.L. 114-315) extended this time period to be 10-years (i.e., to 2024).91 The VA intends to allocate the new residency positions by 2023. This expansion began in academic year (AY) 2015, when the VA allocated 204.3 new VA positions; the largest number of positions were from primary care (73.8 positions) and mental health care (57.8 positions).92 Positions were allocated to 82 facilities in 38 states (positions were also allocated to facilities in the District of Columbia and Puerto Rico). As of July 1, 2015, about 162.9 of the 204.3 allocated positions were filled.93 To support residents training beginning in AY2016, the VA allocated 167.99 new VA positions and 175.2 positions to support residents beginning training in AY2017, for a cumulative three-year total of 547.41. The largest number of positions overall were from internal medicine (191.42) and psychiatry (117.17). Positions were allocated in 38 states.94
The recently enacted John S. McCain III, Daniel K. Akaka, and Samuel R. Johnson VA Maintaining Internal Systems and Strengthening Integrated Outside Networks Act of 2018, or the "VA MISSION Act of 2018" (P.L. 115-182), included a provision to establish a new pilot program for GME in underserved areas.95 The program has not yet been implemented. The new pilot program will create the medical residency positions authorized under the Veterans Access, Choice, and Accountability Act (38 U.S.C.§ 7302 note) at facilities operated by the Indian Health Service, or by Indian Tribes, a federally qualified health center (FQHC),96 a DOD facility, or another facility that the VA Secretary deems appropriate. During the pilot program, the Secretary is required to place no fewer than 100 residents in these facility types or at facilities located in areas that are deemed underserved by criteria established in the VA MISSION Act of 2018. The pilot program authorizes the VA Secretary to pay resident stipends and benefits regardless of whether the resident has been assigned to a VA facility. For facilities that establish new residency programs, the VA will pay for the costs associated with doing so including curricula development, faculty salaries, faculty and resident recruitment, costs associated with the program becoming accredited, and resident educational expenses. This pilot program will terminate on August 7, 2024.
Health Resources and Services Administration
The Health Resources and Services Administration (HRSA) supports GME primarily through two programs: Children's Hospital GME program (CHGME) and the teaching health center GME (THCGME). The CHGME program trains both general pediatricians and pediatric subspecialists, while the THCGME trains residents in outpatient settings in primary care and psychiatry. In addition to these ongoing programs, in FY2019, HRSA received appropriations to support two GME related programs. Under the first, the agency received $25 million to provide grants to public institutions of higher education in states with primary care provider shortages to expand or support GME. These grants will be for five years (as of this report's publication, no funding announcement has been released).97 Under the second program, HRSA received $10 million to support the Rural Residency Development program, which provides funds to award to entities, such as rural hospitals or FQHCs to develop "rural training tracks." This funding builds on an FY2018 appropriation of $15 million to support this program. Rural training tracks are residency programs where residents spent a portion of their early training at an urban hospital and then complete their training in a rural area. Programs meeting certain criteria may be exempt from the Medicare GME cap, but GAO noted that entities interested in starting these programs may not do so because Medicare funds are only available after residents begin training.98 This grant program provides start-up funds for entities to develop the GME programs.99
HRSA also supports residency training through several smaller programs that do not focus explicitly on residency training but permit residency support as one of the allowable uses of funds.100 Through these programs, in AY2016-2017, HRSA supported 2,098 primary care residents101 and 130 preventive medicine residents.102 In addition to these programs, some residents may receive training in community-based settings supported by the Area Health Education Center (AHEC) Program or may receive specialized training in geriatrics through the Geriatric Workforce Enhancement Program. Data on the number of medical or dental residents trained through the AHEC and geriatrics program are not available; rather, available data are on all post-graduate health professionals trained in these programs.103
Children's Hospitals GME104
The Children's Hospitals GME (CHGME) payment program is a discretionary program created in 1999105 and most recently reauthorized through FY2023 in P.L. 115-241.106 The program received an appropriation of $325 million in FY2019107 to provide direct financial support to 58 free-standing children's hospitals108 to train pediatricians and pediatric subspecialists. CHGME was created because children's hospitals typically received little, if any, Medicare GME payments because Medicare's GME payments are made based on a hospital's Medicare patient volume, which is generally low at children's hospitals because Medicare beneficiaries are individuals aged 65 and over, individuals receiving Social Security Disability Insurance benefits, and individuals with end-stage renal disease (i.e., permanent kidney failure).
At the time the CHGME program was created, advocates argued that the lack of direct federal support for GME in children's hospitals impeded the development of the pediatric workforce because children's hospitals, rather than general hospitals, are more likely to have the patient volume necessary to train pediatric subspecialists.109 Since the CHGME program's creation, the overall size of the pediatric and pediatric subspecialty workforce has increased, whereas it had been declining in the 1990s before the program began. Advocates argue that this reverse can be attributed to the CHGME program, because nearly half of all pediatric residents and nearly two-thirds of all pediatric subspecialty fellows train at children's hospitals.110 Others argue that children's hospitals do not need these subsidies because they have fewer uninsured patients than do general hospitals so they should be able to support training without these subsidies.111
The CHGME program makes both DGME and IME payments to children's hospitals for residents and fellows in training. It allocates one-third of its appropriation to DGME payments and the remaining two-thirds to IME payments. During academic year 2016-2017, the program supported 7,164 FTE residents.112 This includes support for 5,017 general pediatric residents, including residents from combined pediatrics programs (e.g., internal medicine/pediatrics). In addition, the program supported training 2,713 pediatric medical subspecialty residents, 285 pediatric surgical subspecialty residents, and 365 pediatric dentistry residents. The program's funds also supported 3,120 adult medical and surgical specialty residents, such as those training in family medicine residents who rotate through children's hospitals for pediatrics training.113
The program must make payments to all children's hospitals that meet the program's definition and have an eligible training program. Therefore, as the number of children's hospitals or eligible training programs increases, the program will provide lower payment levels per resident, unless the amount of funding appropriated to the program increases. This also means that HRSA does not have the authority to use this program to affect the geographic distribution of pediatric trainees.
Unlike CMS programs, HRSA does require CHGME funding recipients to report data on a number of program elements. They are required to report financial data; specifically, they must detail the support they receive from other sources to prevent duplication of payment and programs are required to return duplicate payments.114 CHGME programs are also required to report programmatic data including data on the number of residents they train, the specialties they train in, and whether individuals who complete their training care for children within the hospital's service area or state.115 HRSA also uses these data to track former trainees as they progress in their careers to examine outcomes such as whether these trainees serve patients who are covered by Medicaid.116
The 2013 program reauthorization also includes a new authority for HRSA to develop a quality bonus system where a percentage of the program's appropriation is reserved and then allocated to hospitals that meet specified quality targets. The program is collecting baseline data in FY2019 about CHGME resident involvement in hospital quality initiatives (e.g., integrated care models and social determinants of health). These data will be used as a baseline to establish standards for implementation in FY2021.117
Teaching Health Center GME
HRSA administers the teaching health center GME program (or THCGME), which provides payments to outpatient facilities to support the training of primary care medical and dental residents at these facilities.118 Because residency training has been, in general, hospital-based, experts have raised concerns that physicians are not prepared to treat patients in outpatient settings, where care is increasingly being delivered.119 Under the THCGME program, HRSA provides DGME and IME payments to outpatient facilities, such as federal health centers (a.k.a. FQHCs),120 to support the costs associated with residency training. The program started in FY2011, supporting residents who began their training in AY2012. The program has been funded by direct appropriations enacted in three successive laws: (1) the ACA, which provided funding from FY2011-FY2015; (2) the Medicare Access and CHIP Reauthorization Act of 2015, which provided funding for FY2016 and FY2017 (P.L. 114-10); and (3) the Bipartisan Budget Act of FY2018 (P.L. 115-123), which provides funding for FY2018 and FY2019.121 The most recent extension included expanded program funding to both increase the number of training programs operating and the number of trainees supported at existing programs.122 Table 3 shows the program's funding and number of residents trained since its inception.
|
Academic Year |
Number of Residents (Full-Time Equivalents) Funded |
Total Number of Residents Trained |
Number of Residency Programs Funded |
Funding Source |
|
2011-2012 |
63 |
N/A |
11 |
ACAa |
|
2012-2013 |
143 |
158 |
22 |
ACAa |
|
2013-2014 |
327 |
361 |
44 |
ACAa |
|
2014-2015 |
556 |
600 |
60 |
ACAa |
|
2015-2016 |
660 |
758 |
60 |
MACRAb |
|
2016-2017 |
742 |
771 |
59 |
MACRAb |
|
2017-2018 |
800c |
N/A |
56d |
BBA2018e |
|
Total |
2,623f |
2,648g |
—h |
Source: CRS Analysis of various years of Budget Justifications from the Health Resources and Services Administration (HRSA).
Notes: ACA = The Patient Protection and Affordable Care Act (P.L. 111-148, as amended). MACRA = Medicare Access and CHIP Reauthorization Act of 2015 (P.L. 114-10). BBA 2018 = Bipartisan Budget Act of FY2018 (P.L. 115-123). N/A = not available.
a. ACA provided $230 million for FY2011-FY2015.
b. MACRA provided $60 million for each of FY2016-FY2017. The FY2017 amount was reduced to $55.9 million.
c. Number included in the HRSA FY2019 Budget Justification. This number was estimated prior to the BBA 2018 enactment; as such, this estimate does not account for the program's funding extension or the increased funding that was included in BBA 2018.
d. CRS Analysis of HRSA Grants data obtained from http:data.HRSA.gov.
e. BBA 2018 provided $126.5 million for each of FY2018 and FY2019.
f. Includes the number anticipated in 2017-2018; excluding these residents, the program has funded 1,823 residents.
g. Total for years where data are available.
h. Given that medical residency training is a multiyear process, the same program participates in the THCGME program in multiple years. As such, the data in the table should not be summed to obtain a total number of programs that have participated in the program. In addition, some grantees may operate multiple training program (e.g., a training program in family medicine and another in psychiatry).
HRSA awards THCGME funds to all facilities eligible for payments under the statutory definition of a teaching health center.123 In statute, the program's funds must be used to support primary care residents (defined as residents training in family medicine, internal medicine, pediatrics, combined training in internal medicine-pediatrics, obstetrics and gynecology, psychiatry, general dentistry, pediatric dentistry, or geriatrics).124 Programs were paid $150,000 per FTE under the ACA funding, and $95,000 per FTE using the MACRA funds. This decrease occurred because there are now more residents in training than when the program began. The program's per resident funding level under BBA 2018 is not yet known; however, a 2015 survey of active programs by HRSA indicate that the cost of training a resident at a teaching health center was $157,602 per resident. This amount is higher than estimated in other programs, in part, because THGME programs are small, which lessens economies of scale and because the programs estimate higher costs for training in outpatient facilities. 125 To determine the cost of training at THCs, HRSA contracted with George Washington University to develop a THCGME cost reporting instrument to better reflect the costs that THCs incur when operating GME programs. The instrument includes both the costs that THCs incur while training and the revenues that residents generate. Though some THCs had challenges reporting all of the data elements, this information provided a more comprehensive accounting of costs than are available for most federally support GME programs.126
The THCGME program is required to collect data on various aspects of the residents it trains and the BBA 2018 included additional data collection requirements. Specifically, it required HRSA to report on (1) the number of patients treated by THC residents; (2) the number of visits by patients treated by THC residents; and (3) the number of THC residents who completed a residency in the reporting year, and the number and percentage of these residents who (1) entered primary care practice and (2) entered practice at a health care facility in a HPSA or a rural area. Finally, the law requires the HHS Secretary to submit a report to Congress, by March 31, 2019, on the costs that THCs incur while training residents.
The first THCGME class completed it training in 2014; as such, outcomes associated with the program are preliminary. HRSA's data suggest that the program is successful at training residents who enter primary care and that its graduates are more likely to enter into primary care practice at safety net facilities (such as the facility types that are eligible to sponsor a THCGME program).127 Follow-up studies showed that 69% of all THCGME graduates were currently practicing in a primary care setting and 55% were in a medically underserved community and/or rural setting.128
Department of Defense (DOD)
The Department of Defense (DOD) trains residents who have acquired a uniformed service obligation through a DOD physician training program. Examples include the Uniformed Services University of the Health Sciences (USUHS)129 and the Health Profession Scholarship Program. USUHS students enter active uniformed service as medical students, receive the pay and benefits of an officer at the O-1 level, and incur a seven-year service obligation upon graduation. Under the scholarship program, DOD pays tuition and fees, plus a monthly stipend for students enrolled in civilian medical schools. In return, the students incur an obligation to serve a year of active duty service for each year of benefits received, with a two-year minimum obligation. Upon graduation, most scholarship program participants (regular program participants) go on active duty and begin GME in military hospitals. Other scholarship program participants (deferred program participants) are granted deferments while they pursue civilian GME.
In FY2017, DOD administered residency programs at 26 DOD hospitals and trained an estimated 1,455 FTE residents in over 100 specialties.130 DOD residency programs are accredited by ACGME and managed by each respective military service. The military services generally partner with civilian teaching hospitals, where residents rotate for training in areas or populations not seen at a DOD hospital. Residents from civilian partner facilities may also rotate to DOD facilities. DOD exercises control over the type of residents it trains and the facilities where they train. Specifically, each of the military services determines its workforce requirements and then coordinates with the DOD Comptroller to ensure adequate funding.
Within the Army, the GME Program Office in the Medical Education Directorate of the Office of The Surgeon General develops policy, manages the tri-service Medical Occupation Data System GME database, serves as the Army primary point of contact for GME, and coordinates the Army responsibilities for an annual selection board. The number, specialty, and location of specific training program slots are specified in an annual school year plan approved by the Surgeon General of the Army that serves as a blueprint for the Joint Services GME Selection Board (JSGMESB). This board convenes annually to select trainees for all programs.
Within the Air Force, the number and specialty type of training slots are determined through the Air Force Health Professions Education Requirements Board (HPERB). This annual process models expected attrition, identifies health care workforce needs, and plans and programs for GME needs. The HPERB receives GME training requests from medical commands each March. Since Air Force medical billets are frequently integrated into sister service facilities, the Air Force commands collaborate with the other services in developing these requests.
Within the Navy, the Chief of the Navy Medical Corps determines the number and specialty of training slots during an annual training plan meeting. Input from manpower and personnel planners, clinical specialty leaders, and the Office of the Chief of the Navy Medical Corps are used in developing the annual Training Plan. Similar to the other services, the process culminates in selections made at the annual JSGMESB.
Because many DOD training programs are either integrated or collocated, the service GME chiefs collaborate throughout the year to ensure the integrity, efficiency, and quality of the military GME process. This involves aligning training slots to DOD hospitals that have adequately large and diverse patient populations to sustain the training requirements.
GME is funded through the annual DOD appropriation in the Defense Health Program budget account under Operations & Maintenance in the Education and Training budget activity group.131 For FY2018, Congress appropriated $692.6 million for DOD health care education and training. While the GAO estimated in FY2012 that DOD spent $16.5 million on GME,132 the military departments report that attempts to determine the actual cost of GME have been unsuccessful.133 The military departments agree that the data necessary "to do a valid calculation are not available." 134 This assessment is consistent with data collection variances in non-DOD administered GME programs.135
Concluding Observations
The federal government funds a number of programs that support medical residency training. These programs are operated by different departments across the federal government, and each has its own stated program goals. The rules governing these programs and the purposes of federal support vary. These programs have generally not been examined in conjunction with one another and may have goals that are contrary, duplicative, or otherwise not aligned. For example, in a 2015 report, GAO specifically noted that CMS's GME programs (i.e., Medicare and Medicaid) do not target areas that HHS has identified as workforce needs, nor do they align with workforce goals included in HHS's strategic plan.136 A 2018 report GAO issued reconfirmed this finding.137 The Council on Graduate Medical Education (COGME), the federal advisory group tasked with examining GME policy, also noted a lack of alignment across programs and in its 2017 report called for "a national strategic plan for graduate medical education" to be created by a non-partisan strategic planning committee.138
One of the major challenges for GME policymakers is that data to evaluate programs are lacking. This lack of program transparency has been a consistent theme in a number of recent GME evaluations.139 In the 2018 GAO report noted above, GAO found that HHS and VA GME programs did not collect sufficient data to properly evaluate the federal government's GME investments. This report did not evaluate DOD GME. GAO recommended that HHS and the VA identify information needed to evaluate their GME investments and improve the quality and consistency of data collected.140 Their study found among HHS and VA GME programs that the data collection was generally done at the individual program level and was generally collected to determine hospital compliance with program statute and were not sufficient to determine program costs. In addition, because the data collected were to determine compliance with different program statutes, these data were not consistent across programs. GAO did state that collecting GME data may be difficult because some aspects of the costs of GME training are difficult to quantify (e.g., faculty teaching salaries) and that GME costs vary by site (e.g., costs would differ between a hospital and a clinic where residents rotate for training). Despite these challenges, GAO has consistently recommended better data collection for GME programs.141 The HRSA THCGME supported the development of a data collection instrument to quantify both teaching costs and revenue generated by residents. As part of this analysis, they surveyed THC programs to attempt to identify these data elements (including services and space that were donated to programs). Overall, they found that most programs were able to quantify the expenses associated with training, but that examining the revenue generated was more difficult.142 Despite these challenges, the data collection instrument because of its scope might be useful to better quantify the costs of residency training at other facility types and by other payers.143
Although efforts are underway to improve data collection, they are largely at beginning stages and are not coordinated across programs. As mentioned, the CHGME program is collecting baseline data to develop quality measures for its program. As part of the development of standards, HRSA sought public comments. In general, the commenters noted that there were no generally accepted standards for measuring residency program quality, and that the lack of accepted measures made it difficult to judge relative program performance or change over time.144 As such, the agency is collecting baseline data, including detailed curriculum data, in FY2019 and is focusing on hospital quality initiatives that have direct resident involvement. Another effort in its early stages is being undertaken by the National Academy of Medicine, which sought expert input about how to develop metrics to evaluate individual residency program outcomes at a meeting held in 2017. Although workshop participants overall agreed that GME quality measures are needed, most noted that developing and collecting these measures would be challenging. For example, if one of the outcomes of interest is the quality of care that a training program's graduates provide, it is difficult to attribute whether a program graduate's ability to provide quality care is due to the training received during medical school, residency, or from peers while in practice.145 Some academic research has been undertaken in this area, which has shown that residency training can affect the quality of care its residents deliver and the cost of that care.146 Despite progress in this area, efforts are generally preliminary and data available are limited.
The current lack of data (overall or for specific programs) makes it difficult for policymakers seeking to amend GME payments, because data are not available to evaluate the relative success or weakness of the current payment systems. This may be particularly challenging for those who wish to expand payments, because the limited data that do exist indicate that payments—in particular, Medicare's IME payments—are higher than can be empirically justified.147 As such, some argue that Medicare payments should be reduced; this was suggested by the National Commission on Fiscal Responsibility and Reform,148 by CBO in their Options for Reducing the Deficit,149 and in various years of the President's budget, including a proposal in the FY2019 President's Budget.150 Others argue that payments should be expanded to reduce or avert physician shortages,151 though such shortages themselves have been debated.152
Congress may consider using federal GME support to encourage training in specific specialties and may consider doing so by amending how payments are allocated through existing federal programs, as some of these programs (e.g., Medicare and Medicaid) exercise little control over the specialties they support. Researchers have found that when hospitals expand residency training, they tend to do so in specialties where the benefits derived from residents' labor exceed the cost of their training (i.e., it is profitable for the hospital to train additional residents).153 Current data collected on federal programs make it difficult to determine when a hospital requires an incentive (e.g., a payment from a federal program) to operate a residency program or when it is profitable for a hospital to train residents without an incentive.154 Recent research found that it may be cheaper for a hospital to use resident services than to hire nonphysician providers to replace resident labor and that the outcomes provided by resident were similar or better.155
Congress could pursue policy options to encourage additional training in specific specialties, as it has in the past.156 These options have not always been successful because incentives are generally given to the hospital and often measure the specialty when the resident begins training, which may miss residents who choose to subspecialize.157 Designing policies to affect the specialty composition of the future workforce may be also challenging, because residents may move to a different hospital to pursue further training, because GME incentives are given to the hospital but not to residents, and because current specialty needs, shortages, and surpluses may change.
A related challenge is that currently most federal programs pay the same amount for residents across specialties and by year of training (with the exception of fellows). Some have speculated that a hospital's cost of training a resident may differ by specialty or by the year that the resident is in training. The relative cost to a hospital for operating a residency program may also vary by a number of factors, such as the size of the residency program, the specialty of the program, the total number of residency programs that the hospital operates, and the availability and cost of alternative providers who would be needed to replace the resident's labor. Residents may also generate revenue for a hospital directly (e.g., because they provide additional labor) or may do so indirectly (e.g., because the prestige of a teaching hospital may make it more attractive for some patients). Determining these "costs," should they exist, is challenging. In some cases, federal GME program payments may undercompensate a hospital while in other cases program payments may exceed the hospital's costs.158 GAO attempted to examine the cost of training in a 2018 report and found that measuring these costs was difficult and that some costs were difficult to identify. They also noted that the current data collected were not sufficient to identify these costs or to compare them across GME programs.159 In general, the data collected are not sufficient to determine if or when these scenarios occur nor are data available to determine the factors that may affect hospital training costs. Better data on these "costs" may be useful to better target federal GME support.
Congress may also consider policy options that seek to influence the geographical distribution of residents. Such strategies have been pursued in the past; for example, the ACA's redistribution of Medicare-funded residency slots gave preference to hospitals in states with health professional shortage areas and low resident-to-population ratios.160 Successfully implementing policy options to achieve geographic distribution goals have a number of the same challenges that policy options that seek to target the specialty composition of the physician population do. For example, proposed policy changes generally target hospitals and not the residents themselves, which may be not be effective when the desired outcomes are determined by where the residents ultimately choose to practice. In addition, geographic distribution policies may face challenges because some areas that have traditionally trained residents may lose their current levels of support. For example, prior critiques have raised concerns that where current residents are trained is not reflective of where the current population is located. For example, GAO notes that "Medicare GME funding is disbursed based on historical patterns. Therefore, the Medicare-supported residency slots, supported by this Medicare GME funding, are most highly concentrated in northeastern states."161 GAO confirmed this finding in a 2017 report, which examined residency training from 2005 through 2015 and found that the locations remained largely unchanged despite uneven population growth across regions during this time period.162 Given that training sites have been largely static, successful policy options would either need to add total residents (i.e., expand overall support) or would need to implement a drawdown in support, which may be unpopular and may also be a lengthy process because some residents are currently supported in training programs that last a number of years.
Although prior critiques have focused on Medicare's GME support because it is the largest source of GME support,163 program challenges are not limited to Medicare, as other federal sources of GME support have limited data available and some programs have little flexibility in how payments are used.164 As these programs all seek to train physicians and are, at times, training the same physicians, policymakers may be interested in examining these programs in concert to minimize duplication and maximize program alignment.
Appendix A. Additional Resources
Below are resources for readers interested in specific critiques and policy options suggested to reform Graduate Medical Education (GME). Resources are organized alphabetically by the group that has issued the report.
Council on Graduate Medical Education (COGME)
Federal executive branch advisory council that provides ongoing assessment of physician workforce trends and training. For all reports, see http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/index.html.
Council on Graduate Medical Education, Towards the Development of a National Strategic Plan for Graduate Medical Education, Twenty Third Report, Rockville, MD, April 2017, https://www.hrsa.gov/sites/default/files/hrsa/advisory-committees/graduate-medical-edu/reports/April2017.pdf.
Council on Graduate Medical Education, The Role of Graduate Medical Education in the New Health Care Paradigm, Twenty Second Report, Rockville, MD, November 2014, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/22report.pdf.
Council on Graduate Medical Education, Improving Value in Graduate Medical Education Twenty-First Report, August 2013, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/22report.pdf.
Council on Graduate Medical Education, Enhancing Primary Care, Twentieth Report, December 2010, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/twentiethreport.pdf.
Council on Graduate Medical Education, Enhancing Flexibility in Graduate Medical Education Nineteenth Report, September 2007, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/nineteenthrpt.pdf.
Council on Graduate Medical Education, Financing Graduate Medical Education in a Changing Health Care Environment, Fifteenth Report, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/fifteenthreport.pdf.
Government Accountability Office (GAO)
Federal legislative branch agency that evaluates federal programs including those that finance health care and support the physician workforce. For all reports, see www.gao.gov.
U.S. Government Accountability Office, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding, GAO-18-240, 2018, https://www.gao.gov/assets/700/690581.pdf.
U.S. Government Accountability Office, Physician Workforce: Expansion of the Children's Hospitals Graduate Medical Education Payment Program, GAO-18-66R, 2017, https://www.gao.gov/assets/690/688072.pdf.
U.S. Government Accountability Office, Physician Workforce: Location and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, GAO-17-411, May 5, 2017, https://www.gao.gov/assets/690/684946.pdf.
U.S. Government Accountability Office, Health Care Workforce: Comprehensive Planning by HHS Needed to Meet National Needs, GAO-16-17, December 11, 2015, https://www.gao.gov/assets/680/674137.pdf.
U.S. Government Accountability Office, Health Care Workforce: Federally Funded Training Programs in Fiscal Year 2012, GAO-13-709R, August 15, 2013, https://www.gao.gov/assets/660/656960.pdf.
U.S. Government Accountability Office, Graduate Medical Education: Trends in Training and Student Debt, GAO-09-438R, May 4, 2009, http://www.gao.gov/new.items/d09438r.pdf.
Medicare Payment Advisory Commission (MedPAC)
Federal legislative branch advisory commission that evaluates Medicare payment policy, including Medicare's financing of physician training. For all reports, see www.medpac.gov.
MedPAC, "Does It Cost More to Train Residents or to Replace Them?" September 2013, http://www.medpac.gov/docs/default-source/contractor-reports/sept13_residents_gme_contractor.pdf?sfvrsn=0.
Medicare Payment Advisory Commission, Graduate Medical Education Financing: Focusing on Educational Priorities, Report to the Congress: Aligning Incentives in Medicare, Washington, DC, June 2010, Chapter 4, at http://www.med http://www.medpac.gov/documents/reports/Jun10_Ch04.pdf?sfvrsn=0 pac.gov/documents/Jun10_EntireReport.pdf.
Medicare Payment Advisory Commission's June 2009 Report to Congress: Improving Incentives in the Medicare Program, Chapter 1, at http://www.medpac.gov/documents/reports/Jun09_Ch01.pdf?sfvrsn=0.
National Academy of Medicine (Previously Institute of Medicine)
The National Academies of Sciences, Engineering, and Medicine are private, nonprofit institutions that aim to provide expert advice on pressing domestic and international challenges. Work can be funded by government and non-governmental entities. For all reports, see http://www.nationalacademies.org/.
Board on Health Care Services, Health and Medicine Division, The National Academies of Sciences, Engineering, and Medicine, Graduate Medical Education Outcomes and Metrics: Proceedings of a Workshop, Payal Martin, Mariana Zindel, and Sharyl Nass, Rapporteurs (Washington, DC: National Academies Press, 2018).
Committee on the Governance and Financing of Graduate Medical Education; Board on Health Care Services; Institute of Medicine, Graduate Medical Education That Meets the Nation's Health Needs, ed. Jill Eden, Donald Berwick, and Gail Wilensky (Washington, DC: National Academies Press, 2014).
Committee on Implementing a National Graduate Medical Education Trust Fund, Division of Health Care Services, Institute of Medicine, On Implementing a National Graduate Medical Education Trust Fund. (Washington, DC: National Academies Press, 1997).
Appendix B. GME Program Information
|
Program Name |
Program Description |
Funding Type |
Program Controls Over Trainees |
Total Funding |
Uses of Funding |
Number of Trainees |
Cost Per Trainee |
|
Medicare GME Payments SSA §1886h [42 U.S.C. §§1395ww(d(5)(B), 1395ww(h), (k)] (HHS/CMS) |
Medicare payments to teaching hospitals and certain other training sites to cover the direct teaching costs (such as resident salary and fringe benefits, supervisory physician salaries, and space) and the indirect teaching costs (such as the costs of additional services that residents may order, and other expenses). |
Mandatory. |
The number of Medicare-supported residents and per-resident payment amount is capped for each hospital but hospitals determine staffing needs and types of residents with the exception of certain primary care residents. |
Estimates range from $10.3 to $12.5 billion in FY2015.a |
Resident salary, supervisory physician salaries, and space, along with indirect teaching costs (such as the costs of additional services that residents may order and other expenses). |
Estimates range from 85,712 to 87,980 FTE slots (DGME) and 85,578-88,416 FTE slots (IME) in FY2015.a,b, |
Estimates of the average Medicare payment per FTE range from $112,000 to 129,000 in FY2015.a |
|
Medicaid GME Payment (HHS/CMS) |
Medicaid GME payments may also be included as part of capitation rates under managed care. The availability of these payments varies by state. |
Mandatory. |
States are permitted to make these payments to providers using their own criteria. |
N/A. |
States are permitted to determine a provider's appropriate uses of Medicaid GME funding. |
N/A. The Medicaid program does not require states to report these data. |
N/A. The Medicaid program does not require states to report these data. |
|
Veterans Affairs GME Payments [38 U.S.C. §7302]. (VHA/VA) |
Training of medical residents at facilities operated by the VA. |
Discretionary. |
VA facilities determine their staffing needs and the number and type of residents supported. |
$1.78 billion in AY2016-2017. |
Resident salary, supervisory physician salaries, and space. |
11,000 FTE slots and more than 43,565 residents spent part of their training at a VA facility in AY2016-2017. |
$137,792 per resident (estimated in AY2015).c |
|
Children's Hospital GME Payment Program |
Payments to freestanding children's hospitals that sponsor medical residency training programs in pediatrics and pediatric medical and surgical subspecialties in order to increase the number of physicians practicing in those specialties. |
Discretionary. |
Grant funding awarded to applicant children's hospitals that meet the program's eligibility requirements. |
$325 million in FY2019.d |
Funds to hospitals to support trainee stipends, faculty salaries, and program administrative expenses. IME costs associated with operating a program (expenditures associated with reduced hospital efficiency). |
58 hospitals received payments to support 7,164 FTE slots in AY2016-2017. |
N/A |
|
Teaching Health Centers GME Payment Program PHSA §340H [42 U.S.C. §256e] |
Payments to qualified teaching health centers (i.e., community-based facilities that sponsor medical residency programs in primary care or psychiatry or primary care dental residency programs) to support residency training programs. |
Mandatory (funding authorized through FY2019). |
Funding to applicant teaching health centers that meet the program's eligibility requirements. |
$126.5 million in FY2018.e |
Funds to support trainee stipends, faculty salaries, and program administrative expenses. IME costs associated with operating a program (expenditures associated with reduced health center efficiency). |
742 FTE slots and 771 total residents trained in AY2016-AY2017. |
N/A |
|
Department of Defense GME Payments [10 U.S.C. § § 2001 et. seq.] |
Training of medical residents at facilities operated by the DOD. |
Discretionary. |
Divisions of the armed forces determine their staffing needs and the number and type of residents supported. |
$16.5 million in FY2012. |
Resident salary, supervisory physician salaries, and space. |
3,983 FTE residents in FY2017. |
N/A |
Sources: CRS analysis of agency data, including review of various agency budget justification and The Robert Graham Center program data sourced from CMS Medicare hospital cost report data, and GAO report, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding (GAO-18-240, 2018). AY = Academic year; Academic year 2016-2017 began on July 1, 2017, and concluded on June 30, 2017; CMS = Centers for Medicare & Medicaid Services; DGME = direct graduate medical education; DOD = Department of Defense; FTE = full time equivalent; FY = fiscal year; HHS = Department of Health and Human Services; HRSA = Health Resources and Services Administration; IME = Indirect Medical Education; N/A = not available; PHSA = Public Health Service Act; U.S.C. = U.S. Code; VA = Department of Veterans Affairs; VHA = Veterans Health Administration.
a. This range is based on three estimates of FY2015 Medicare GME payments. One estimate is calculated and published by GAO (GAO-18-240, 2018, https://www.gao.gov/assets/700/690581.pdf). A second estimate is based on a CRS calculation using GME payment data published by the Robert Graham Center, a policy research center that provides analysis for physicians and the American Academy of Family Physicians. A third estimate is calculated by CRS using CMS-published hospital cost report data.
b. Trainee numbers are not unduplicated (i.e., DGME and IME payments support the same residents). The total number of FTEs supported differs because DGME and IME count residents differently. For example, DGME payments, but not IME payments, take into account whether or not a resident is in an initial residency program or a fellowship program when counting residents.
c. Data provided by Department of Veterans Affairs, Veterans Health Administration, Office of Academic Affiliations, personal communication with CRS on August 4, 2018.
d. Under P.L. 115-245.
e. Under P.L. 115-123.
Author Contact Information
Acknowledgments
Kenneth Fassel, CRS research assistant, provided support for this report. Katherine M. Kehres, Presidential Management Fellow, and Scott Talaga and Don Jansen, former CRS analysts, also contributed to this report.
Key Policy Staff
|
Area of Expertise |
Name |
|
Health Workforce Data |
Elayne Heisler |
|
Medicare GME |
Marco Villagrana |
|
Medicaid GME |
Alison Mitchell |
|
VA GME |
Sidath Panangala |
|
DOD GME |
Bryce Mendez |
|
HRSA GME (Teaching Health Centers and Children's Hospital GME) |
Elayne Heisler |
Footnotes
| 1. |
U.S. Government Accountability Office (GAO), Health Care Workforce: Comprehensive Planning by HHS Needed to Meet National Needs, 16-17, December 11, 2015, http://www.gao.gov/products/GAO-16-17; hereinafter, GAO Health Workforce Planning Report. |
| 2. |
Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation, Building the Nation's Health Care Workforce, Washington, DC, July 2, 2015. |
| 3. |
Ibid. See also, U.S. Department of Health and Human Services, Health Resources and Services Administration (HRSA), "Shortage Designation: Health Professional Shortage Area & Medically Underserved Areas/Populations," http://www.hrsa.gov/shortage/index.html; and U. S. Department of Health and Human Services, Centers for Medicare & Medicaid Services (CMS), "Physician Bonuses," https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/HPSAPSAPhysicianBonuses/index.html?redirect=/hpsapsaphysicianbonuses/. |
| 4. |
GAO Health Workforce Planning Report. GAO used data from FY2014 for these calculations and GAO's GME data include GME obligations incurred to train certain non-physician providers (e.g., nurses and allied health professionals); however, expenses incurred to train non-physician providers comprise approximately 2% of the agency's overall GME obligations. |
| 5. |
For example, one study found that more than half of physicians who complete their residency in family medicine (a type of primary care) practice within 100 miles of where they trained. See E. Blake Fagan et al., "Migration After Family Medicine Residency: 56% of Graduates Practices Within 100 Miles of Training," American Family Physician, vol. 88, no. 10 (November 15, 2013), p. 704. |
| 6. |
Ibid. |
| 7. |
For example, Medicare's GME payments can be used to support hospital-based training of dentists, podiatrists, nurses, and some allied health professionals. |
| 8. |
GAO, Graduate Medical Education: Trends in Training and Student Debt, 09-438R, May 4, 2009; hereinafter, GAO GME Report. |
| 9. |
Sarah E. Brotherton and Sylvia I. Etzel, "Graduate Medical Education, 2016-2017," Journal of the American Medical Association, vol. 318, no. 23 (December 19, 2017), pp. 2368-2387. |
| 10. |
Ibid. |
| 11. |
GAO GME Report. |
| 12. |
The Accreditation Council for Graduate Medical Education (ACGME) accredits the majority of residency programs; the remaining programs are accredited by the American Osteopathic Association (AOA). The two organizations are transitioning to a single accreditation system. See "Single Accreditation System for AOA-Approved Programs," at http://www.acgme.org/acgmeweb/. In ACGME's Academic Year 2017-2018 Databook, they reported accrediting a total of 11,214 programs (some programs may still be accredited by the AOA and some programs may be jointly accredited). They reported that the number of accredited programs is increasing, but that this increase is primarily driven by programs formerly accredited by AOA seeking ACGME accreditation. ACGME, Data Resource Book: Academic Year 2017-2018, Chicago, IL, 2018, pp. 11-12. |
| 13. |
Federal funds are not the only source available for GME. For example, state and local governments could pay for GME and hospitals could use their revenue for GME. Data are not available on the full amount expended for GME (i.e., no data exist that aggregate the cost paid for GME by the federal government and other payers). |
| 14. |
Committee on the Governance and Financing of Graduate Medical Education; Board on Health Care Services; Institute of Medicine, Graduate Medical Education That Meets the Nation's Health Needs, ed. Jill Eden, Donald Berwick, and Gail Wilensky (Washington, DC: National Academies Press, 2014); hereinafter, 2014 IOM GME Report and GAO, Health Care Workforce: Federally Funded Training Programs in Fiscal Year 2012, 13-709R, August 15, 2013; hereinafter, GAO Health Care Workforce Report. The IOM's estimates are for physician residency and fellowship training. This report uses data from multiple years because more recent data are available for some, but not all, GME programs. |
| 15. |
GAO Health Care Workforce Report, p. 5. |
| 16. |
GAO Health Workforce Planning Report. |
| 17. |
Generally, the federal government leaves the content of training to the accrediting bodies. However, federal advisory groups have made recommendations on topics to add to training, and the federal government awards grants for certain types of training experiences. As examples, the Council on Graduate Medical Education (COGME) has recommended that medical residents learn how to work in a medical home model (see, for example, COGME, The Role of Graduate Medical Education in the New Health Care Paradigm, Twenty Second Report, Rockville, MD, November 2014, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/22report.pdf), and HRSA awards grants for training in geriatrics (see http://bhpr.hrsa.gov/grants/geriatricsalliedhealth/index.html). |
| 18. |
The Medicare Payment Advisory Commission (MedPAC) June 2009 Report to Congress: Improving Incentives in the Medicare Program, Chapter 1, at http://www.medpac.gov/chapters/Jun09_Ch01.pdf; hereinafter 2009 MedPAC Report. GAO also noted that Medicare's support of GME was not linked to other workforce programs and did not have the oversight and infrastructure to track the outcome of its GME investments; see GAO Health Workforce Planning Report. |
| 19. |
Estimates based on CRS analysis of FY2015 Medicare hospital cost report data as reported to the CMS Healthcare Cost Report Information System; figures reported by GAO, Physician Workforce: HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding, GAO-18-240, 2018, p. 50, https://www.gao.gov/assets/700/690581.pdf; herein after, GAO 2018 GME Information; and CRS analysis of Medicare cost report-based data published by The Robert Graham Center, https://www.graham-center.org/rgc/maps-data-tools/data-tables/gme.html. Also, see "Different Estimates of Medicare GME Payments and FTEs" discussion in the "Medicare" section of this report. |
| 20. |
For more information on Medicare GME limits, see "Medicare DGME Payments" section of this report. |
| 21. |
GAO, Physician Workforce: Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, 17-411, May 25, 2017. |
| 22. |
Barbara O. Wynn, "Is the Teaching Health Center Graduate Medical Education Program a Model for GME Reform?" Journal of Graduate Medical Education, vol. 10, no. 2 (April 2018), pp. 165-167. |
| 23. |
Edward Salsberg et al., "U.S. Residency Training Before and After the 1997 Balanced Budget Act," Journal of the American Medical Association, vol. 300, no. 10 (September 10, 2008), pp. 1174-1180. |
| 24. |
For example, the Association of American Medical Colleges (AAMC), the organization that represents medical schools and teaching hospitals, has argued that the Medicare GME cap is detrimental to medical training and leads to geographic and specialty shortages. See AAMC, "Medicare Resident Limits ('Caps')," https://www.aamc.org/advocacy/gme/71178/gme_gme0012.html. |
| 25. |
For example, in the 115th Congress, legislation has been introduced that would expand Medicare GME support, see, for example, H.R. 2267, S. 1301, H.R. 284 and H.R. 6056. |
| 26. |
See, for example, discussion in Edward S. Salsberg, "Is the Physician Shortage Real? Implications for the Recommendations of the Institute of Medicine Committee on the Governance and Financing of Graduate Medical Education," Academic Medicine, vol. 90, no. 9 (September 2015), pp. 1-5. |
| 27. |
GAO, Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, 17-411, May 25, 2017. |
| 28. |
See, for example, National Center for Health Workforce Analysis, HRSA, Distribution of U.S. Health Care Providers Residing in Rural and Urban Areas, Rockville, MD, October 2014, http://bhpr.hrsa.gov/healthworkforce/supplydemand/nchwafactsheet.pdf. In addition, private organizations such as the American Medical Association collect data on the number of physicians. |
| 29. |
HRSA, Bureau of Health Workforce, Health Workforce Analysis "Projecting the Supply and Demand for Primary Care Practitioners Through 2020: In Brief," November 2013, http://bhpr.hrsa.gov/healthworkforce/supplydemand/usworkforce/primarycare/index.html. |
| 30. |
CRS In Focus IF10322, Medicaid Primer. |
| 31. |
Congressional Budget Office, Repealing the Individual Health Insurance Mandate: An Updated Estimate, Washington, DC, November 2017, https://www.cbo.gov/system/files?file=115th-congress-2017-2018/reports/53300-individualmandate.pdf and Congressional Budget Office, Federal Subsidies for Insurance Coverage for People Under Age 65: 2018 to 2028, May 2018, https://www.cbo.gov/system/files/115th-congress-2017-2018/reports/53826-healthinsurancecoverage.pdf. |
| 32. |
HRSA, Bureau of Health Workforce, Health Workforce Analysis "Projecting the Supply and Demand for Primary Care Practitioners Through 2020: In Brief," November 2013, http://bhpr.hrsa.gov/healthworkforce/supplydemand/usworkforce/primarycare/index.html. |
| 33. |
Tim Dall et al., 2017 Update: The Complexities of Physician Supply and Demand: Projections from 2015 to 2020, IHS Markit Prepared for the Association of American Medical Colleges, Final Report, Washington, DC, February 28, 2017. |
| 34. |
David I. Auerbach et al., New Approaches for Delivering Primary Care Could Reduce Predicted Physician Shortages, Research Highlight,, Rand Corporation, Research Briefs RB9752, 2013, http://www.rand.org/pubs/research_briefs/RB9752.html. |
| 35. |
In FY2017, there were 6,900 areas designated as having a primary care shortage. See HRSA, "HRSA Fact Sheet: FY2017- Nation" at https://data.hrsa.gov/data/fact-sheets. |
| 36. |
GAO, Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, 17-411, May 25, 2017. |
| 37. |
See, for example, simulations undertaken using the FutureDocs Forecasting tool. Emily K. Tierney et al., FutureDocs: Nation Has Enough Physicians to Meet the Nation's Overall Needs—For Now. Distribution to Worsen, The Cecil C. Sheps Center for Health Services Research, The University of North Carolina at Chapel Hill, Issue Brief #1, Chapel HIll, NC, April 26, 2017. |
| 38. |
This uncertainty was one of the major reasons that the IOM did not recommend increasing the amount of GME funding; see 2014 IOM GME Report. Others have also argued that because not all states have implemented the ACA's Medicaid expansion, more local projections may be required because the need for physicians (and other health services) varies by area. See Rob Cunningham, Challenges of Forecasting Physician Workforce Needs Amid Delivery System Transformation, National Health Policy Forum, Issue Brief No. 851, Washington, DC, September 29, 2015. |
| 39. |
GAO, Health Care Workforce: Comprehensive Planning by HHS Needed to Meet National Needs, 16-17, December 11, 2015, http://www.gao.gov/products/GAO-16-17 and GAO 2018 GME Information. |
| 40. |
For example, see CRS Report R43571, Federal Student Loan Forgiveness and Loan Repayment Programs, and CRS Report R44970, The National Health Service Corps. |
| 41. |
GAO Health Workforce Planning Report. This estimate includes support for other health professions beyond physicians; however, support for physicians is the largest component of GME. |
| 42. |
The Medicare program is a federal program that pays for covered health care services for qualified beneficiaries. Medicare beneficiaries are individuals aged 65 and over, individuals receiving Social Security Disability Insurance benefits, and individuals with end-stage renal disease (i.e., permanent kidney failure). For more information on the Medicare Program, see CRS Report R40425, Medicare Primer. |
| 43. |
U.S. Congress, House Committee on Ways and Means, Social Security Amendments of 1965, 89th Cong., 1st sess., March 29, 1965, House Report No. 213 (Washington: GPO, 1965), p. 32. |
| 44. |
This range is based on three estimates of FY2015 Medicare GME payments. One estimate is calculated and published by GAO (GAO-18-240, 2018, https://www.gao.gov/assets/700/690581.pdf). A second estimate is based on CRS calculation of GME payment data published by the Robert Graham Center, a policy research center that provides analysis for physicians and the American Academy of Family Physicians. A third estimate is calculated by CRS using CMS-published hospital cost report data. CRS analyzed FY2015 Medicare hospital cost report data as reported to CMS's Healthcare Cost Report Information System. This figure does not include Medicare's medical education payment adjustments for psychiatric hospitals and rehabilitation hospitals that operate teaching programs since the bulk of Medicare GME payments and the Medicare GME policies described in this report apply to general acute care hospitals that are paid under the Medicare inpatient prospective payment system (IPPS). |
| 45. |
See The Graham Center, "GME Table User Guide and Frequently Asked Questions," https://www.graham-center.org/content/dam/rgc/documents/maps-data-tools/gme_teaching_hospitals/GMEtablesuserguide.pdf. |
| 46. |
MedPAC, in its 2009 report, noted that despite Medicare' role in GME payments it has never used these payments to affect changes in medical education or the workforce. See MedPAC 2009, pp. 19. |
| 47. |
U.S.C. §1395ww(h). Generally, the federal government leaves the content of training to the accrediting bodies. However, federal advisory groups have made recommendations on topics to add to training, and the federal government awards grants for certain types of training experiences. As examples, the COGME has recommended that medical residents learn how to work in a medical home model (see, for example, COGME, The Role of Graduate Medical Education in the New Health Care Paradigm, Twenty Second Report, Rockville, MD, November 2014, http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/22report.pdf), and the HRSA awards grants for training in geriatrics (see http://bhpr.hrsa.gov/grants/geriatricsalliedhealth/index.html).See also, GAO Health Workforce Planning Report. |
| 48. |
CMS gathers resident and specialty data from teaching hospitals using the Intern and Resident Information System (IRIS). See GAO 2018 GME Information. |
| 49. |
AAMC, Medical Education and Residency Issues, Consensus Statement on Physician Workforce, March 3, 1997. |
| 50. |
The Medicare allopathic and osteopathic resident limit does not apply to critical access hospitals (small rural hospitals with no more than 25 inpatient beds), which are reimbursed for GME based on 101% of the reasonable costs incurred. |
| 51. |
AAMC, Medicare Payments for Graduate Medical Education: What Every Medical Student, Resident, and Advisor Needs to Know, January 2013. |
| 52. |
The Medicare cap does not preclude hospitals from training residents beyond the FTE slots capped under Medicare based on 1996 levels using other funding. |
| 53. |
The Medicare cap for new residency training programs is based on the sum of the products of the highest number of FTE residents in any program year during the fifth year of the new program's existence and the number of years in which residents are expected to complete the program based on the minimum accredited length for each type of program. For more information on the cap for newly-created training programs, see 42 CFR 413.79(e). |
| 54. |
Edward Salsberg et al., "U.S. Residency Training Before and After the 1997 Balanced Budget Act," Journal of the American Medical Association, vol. 300, no. 10 (September 10, 2008), pp. 1174-1180 and GAO, Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, GAO-17-411, May 25, 2017. |
| 55. |
Barbara O. Wynn, "Is the Teaching Health Center Graduate Medical Education Program a Model for GME Reform?" Journal of Graduate Medical Education, vol. 10, no. 2 (April 2018), pp. 165-167. |
| 56. |
For example, GAO estimates that under the ACA-authorized, one-time redistribution of unused slots, 599 unused IME and 692 unused DGME resident FTEs were transferred to approximately 51 other hospitals, effective July 1, 2011. For more information about Medicare GME slot redistribution programs, see https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/DGME.html. |
| 57. |
These figures reflect CRS-calculated estimates. For additional information about different sources of GME payments and FTEs, see the "Different Estimates of Medicare GME Payments and FTEs" text box in the "Medicare" section of this report, and Table 1 and Table B-1 in Appendix B. |
| 58. |
Some operators of GME programs contend that DGME costs are too low and do not reflect the direct costs that a hospital incurs when operating a residency program. For example, one hospital president estimated that DGME was nearly $40,000 too low per-resident per-year and that IME payments were used to (among other things) offset the DGME underpayment. See Marc L. Bloom, "Graduate Medical Education," Institute of Medicine, "Understanding the Costs and Financing of GME," Washington, DC, December 20, 2012, http://iom.nationalacademies.org/~/media/Files/Activity%20Files/Workforce/GMEGovFinance/2012-DEC-19/Boom.pdf. The AAMC also analyzed FY2009 Medicare hospital cost reports and noted that DGME payments reimbursed less than one-quarter of the total direct costs incurred by the teaching hospital. See U.S. Congress, Senate Committee on Health, Education, Labor, and Pensions, Subcommittee on Primary Health and Aging, 30 Million New Patients and 11 Months to Go: Who Will Provide Their Primary Care?, Statement for the Record by the Association of American Medical Colleges, 113th Cong., 1st sess., January 29, 2013, p.2. |
| 59. |
Following the enactment of the Consolidated Omnibus Budget Reconciliation Act of 1985 (P.L. 99-272), Medicare DGME payments would not be open-ended but based on the hospital's DGME costs in a base period (FY1984 for most hospitals), updated for inflation each year. If a hospital did not have an approved medical residency training program or did not participate in Medicare during the base period, the per-resident amount is established based on a hospital's costs during the first year that the hospital participates in Medicare and the residents who are on duty during the first month of that period. |
| 60. |
The 14% reduction for inpatient days associated with beneficiaries enrolled in Medicare Part C reflects Medicare expenditures that are carved out to make payments to hospitals operating approved nursing or allied health education programs. The nursing and allied health education program and funding mechanism are authorized by section 541(b) of the Medicare, Medicaid, and SCHIP Balanced Budget Refinement Act of 1999 (P.L. 106-113). |
| 61. |
These figures reflect CRS-calculated estimates. For additional information about different sources of GME payments and FTEs, see the "Different Estimates of Medicare GME Payments and FTEs" text box in the "Medicare" section of this report, and Table 1 and Table B-1 in Appendix B. |
| 62. |
In contrast to research that suggests DGME payments do not adequately cover direct costs, MedPAC, among others, contends that IME payments are too high and estimates that IME payments are nearly twice the amount that can be empirically justified For more information, see MedPAC, Report to the Congress: Medicare Payment Policy, March 2007, p.45, http://www.medpac.gov/documents/reports/Mar07_Ch02a.pdf?sfvrsn=0 and MedPAC, Report to the Congress: Medicare Payment Policy, March 2016, http://www.medpac.gov/docs/default-source/reports/march-2016-report-to-the-congress-medicare-payment-policy.pdf?sfvrsn=0. |
| 63. |
See Section 1886(d)(5)(B) of the Social Security Act. |
| 64. |
Medicare IPPS payments consist of two components, one covers hospital operating costs—primarily labor and supply costs—the other covers capital costs such as costs for depreciation, interest, rent, and property-related insurance and taxes. |
| 65. |
Medicaid is a means-tested entitlement program that finances the delivery of primary and acute medical services, as well as long-term services and supports. For more information about the Medicaid program, see CRS Report R43357, Medicaid: An Overview. |
| 66. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016. |
| 67. |
While no federal guidance speaks to Medicaid GME payments, federal regulations specify upper payment limits (UPLs) for Medicaid payments to hospitals, which prohibit using federal matching funds for Medicaid fee-for-service payments in excess of what would have been paid under Medicare payment principles (42 C.F.R. 447.272). Also, states are allowed to include Medicaid GME payments in managed care capitation payments (42 C.F.R. 438.6). |
| 68. |
Under the fee-for-service delivery system, health care providers are paid by the state Medicaid program for each service provided to a Medicaid enrollee. Under the managed care delivery system, Medicaid enrollees get most or all of their services through an organization under contract with the state. |
| 69. |
States submit the CMS-64 form to the Centers for Medicare & Medicaid Services on a quarterly basis, and the CMS-64 form is a statement of expenditures for which states are entitled to federal Medicaid matching funds. States are required to provide supporting documentation for total Medicaid expenditures. |
| 70. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016. |
| 71. |
GAO, Physician Workforce HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding, GAO-18-240, March 2018. |
| 72. |
For most states, the state fiscal year begins on July 1 and ends on June 30 of the following calendar year, whereas a federal fiscal year begins on October 1 and ends on September 30 of the following calendar year. |
| 73. |
Under risk-based managed care, states contract with managed care organizations (MCOs), which are private health insurers. States usually pay the MCOs on a capitated basis, which means the states prospectively pay the MCOs a fixed monthly rate per enrollee to provide or arrange for most health care services. |
| 74. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016; and GAO 2018 GME Information. |
| 75. |
CMS, FY2015 CMS-64 data, as of December 1, 2016. |
| 76. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016; and GAO 2018 GME Information. |
| 77. |
CMS, FY2015 CMS-64 data, as of December 1, 2016; Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016. |
| 78. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016; and GAO 2018 GME Information. |
| 79. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016. |
| 80. |
Tim M. Henderson, Medicaid Graduate Medical Education Payments: A 50-State Survey, AAMC, 2016; and GAO 2018 GME Information. |
| 81. |
GAO 2018 GME Information. |
| 82. |
38 U.S.C. §7302. |
| 83. |
Data provided by Department of Veterans Affairs, Veterans Health Administration, Office of Academic Affiliations, personal communication with CRS on August 4, 2018. |
| 84. |
Ibid. |
| 85. |
Ibid. |
| 86. |
The VA may only reimburse an affiliate to cover the cost for the duration that a medical resident serves in a VA medical facility (Department of Veterans Affairs Veterans Health Administration Disbursement Agreement Procedures for Physician and Dentist Residents VHA HANDBOOK 1400.05 August 14, 2015). |
| 87. |
The VA is affiliated with 144 of 149 allopathic medical schools (MDs) and all osteopathic medical schools (DOs). Data is current for academic year 2016-2017 and may change from year to year. Residency positions do not actually match with VA medical facilities. They match at programs that include the VA medical facility as a participating site. See also CRS Report R43587, The Veterans Health Administration and Medical Education: In Brief. |
| 88. |
Data provided by Department of Veterans Affairs, Veterans Health Administration, Office of Academic Affiliations, personal communication with CRS on August 4, 2018. |
| 89. |
Department of Veterans Affairs, Veterans Health Administration, VHA Handbook, 1400.01, December 19, 2012. |
| 90. |
Ibid. |
| 91. |
CRS Report R43704, Veterans Access, Choice, and Accountability Act of 2014 (H.R. 3230; P.L. 113-146), by Sidath Viranga Panangala et al.; P.L. 114-315; and 38 U.S.C. §7302 note. |
| 92. |
The VA can support partial positions because residents undertake only part of their training at the VA. (Department of Veterans Affairs, Office of Congressional and Legislative Affairs, e-mail communication, July 1, 2015.) |
| 93. |
Office of Academic Affiliations briefing to the Commission on Care, October 6, 2015. |
| 94. |
CRS Report R43587, The Veterans Health Administration and Medical Education: In Brief. |
| 95. |
CRS Report R45390, VA Maintaining Internal Systems and Strengthening Integrated Outside Networks Act of 2018 (VA MISSION Act; P.L.115-182). |
| 96. |
Federally qualified health centers (FQHCs) are often referred to interchangeably with grantees of the federal health center program (health centers or community health centers). These are outpatient primary care-focused facilities that are located in health professional shortage areas. FQHCs may also operate teaching health centers. For more information on these facilities, see CRS Report R43937, Federal Health Centers: An Overview. |
| 97. |
For program details, see discussion of HRSA's Health Workforce programs in Title II of Division A of P.L. 115-245. |
| 98. |
GAO, Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, 17-411, May 25, 2017. |
| 99. |
For more information, see discussion of HRSA's Rural Health programs in Title II of Division A of P.L. 115-245. For the FY2019 Rural Training Track funding announcement, see HRSA, "Rural Residency Planning and Development Program, https://bhw.hrsa.gov/fundingopportunities/default.aspx?id=bd0f561a-78b[phone number scrubbed]-a06f-722afa117f31. |
| 100. |
Information and data about these programs were obtained from HRSA, Justification of Estimates for Appropriations Committees, FY2019, Rockville, MD. |
| 101. |
Public Health Service Act (PHSA) §747. This authority was also used to fund the Primary Care Residency Expansion (PCRE) in FY2010, which provided support to 504 residents. Funding for this program was available only in FY2010, and one study found that residency programs that received funds to train additional residents were not able to keep these positions after the funding period ended. See Melissa Rossan Chen et al., "Are Time-Limited Grants Likely to Stimulate Sustained Growth in Primary Care Residency Training? A Study of the Primary Care Residency Expansion Program," Academic Medicine, vol. 90, no. 9 (September 2015), pp. 1278-1283. |
| 102. |
PHSA §768. |
| 103. |
HRSA, Justification of Estimates for Appropriations Committees, FY2019, Rockville, MD. |
| 104. |
More detailed information about this program, including extensive program data, can be found in CRS Report R45067, Children's Hospitals Graduate Medical Education (CHGME). |
| 105. |
Healthcare Research and Quality Act of 1999 (P.L. 106-129). |
| 106. |
The Children's Hospital GME (CHGME) payment program is authorized in PHSA §340 (42 U.S.C. 256e). |
| 107. | |
| 108. |
PHSA §340E defines a children hospitals as "a hospital with a Medicare payment agreement and which is excluded from the Medicare inpatient prospective payment system pursuant to section 1886(d)(1)(B)(iii) of the Social Security Act and its accompanying regulations." |
| 109. |
The American Academy of Pediatrics, the major professional association for pediatricians, released a 2000 report detailing shortages in pediatric subspecialties and calling for additional financial support for training and research. See Alan Gruskin et al., "Final Report of the FOPE II Pediatric Subspecialists of the Future Workgroup," Pediatrics, vol. 106, no. 5 (November 2000), pp. 1224-1244. |
| 110. |
See, for example, the policy positions of the Children's Hospital Association, "Children's Hospitals Graduate Medical Education Program Overview," https://www.childrenshospitals.org/Issues-and-Advocacy/Graduate-Medical-Education/Issue-Briefs-and-Reports/Childrens-Hospitals-Graduate-Medical-Education-Program-Overview. |
| 111. |
See discussion in CRS Report R45067, Children's Hospitals Graduate Medical Education (CHGME). |
| 112. |
HRSA, Justification of Estimates for Appropriations Committees, FY2019, Rockville, MD. |
| 113. |
Ibid. |
| 114. |
Personal communication, Health Resources and Services Administration, Office of Legislation, June 26, 2015. |
| 115. |
Jim Kaufman, "Understanding the Costs and Financing of GME," Institute of Medicine, panel titled Understanding the Costs and Financing of GME, Washington, DC, December 20, 2012, http://iom.nationalacademies.org/~/media/Files/Activity%20Files/Workforce/GMEGovFinance/2012-DEC-19/Kaufman.pdf. |
| 116. |
National Academy of Medicine, Graduate Medical Education Outcomes and Metrics: Proceedings of a Workshop, Washington, DC, March 27, 2018. |
| 117. |
HRSA, "Proposed Standards for the Children's Hospitals Graduate Medical Education Payment Program's Quality Bonus System," 83 Federal Register 29796-29798, June 26, 2018. |
| 118. |
The program is authorized in PHSA §340H (42 U.S.C. 256h). |
| 119. |
2009 MedPAC Report. |
| 120. |
For information about federal health centers, see CRS Report R43937, Federal Health Centers: An Overview. |
| 121. |
Prior to the enactment of the Bipartisan Budget Act of 2018, the Teaching Health Center GME program received temporary funding extension in the Disaster Tax Relief and Airport and Airway Extension Act of 2017 (P.L. 115-63) and H.R. 1370. Each of these laws provided $15 million for one quarter of FY2018. |
| 122. |
CRS Report R45136, Bipartisan Budget Act of 2018 (P.L. 115-123): CHIP, Public Health, Home Visiting, and Medicaid Provisions in Division E. |
| 123. |
PHSA §749A defines a teaching health center is a community based, ambulatory patient care center that operates a primary care residency program. The definition explicitly includes federal health centers, community mental health centers, rural health clinics, facilities operated by the Indian Health Service, and Title X Family Planning clinics. |
| 124. |
42 U.S.C. §293k. |
| 125. |
HRSA, "Cost Estimates for Training Residents in a Teaching Health Center," https://bhw.hrsa.gov/sites/default/files/bhw/grants/thc-costing-fact-sheet.pdf. |
| 126. |
Marsha Regenstein et al., "Comprehensive Revenue and Expense Data Collection Methodology for Teaching Health Centers: A Model for Accountable Graduate Medical Education Financing," Journal of Graduate Medical Education, vol. 10, no. 4 (April 2018), pp. 157-164 and Barbara O. Wynn, "Is the Teaching Health Center Graduate Medical Education Program a Model for GME Reform?" Journal of Graduate Medical Education, vol. 10, no. 2 (April 2018), pp. 165-167. |
| 127. |
Andrew Bazemore et al., Graduates of Teaching Health Centers are More Likely to Enter Practice in the Primary Care Safety Net, Robert Graham Center, One Pagers, Washington, DC, November 15, 2015, http://www.graham-center.org/rgc/publications-reports/publications/one-pagers/thc-graduates-safety-net-2015.html. |
| 128. |
HRSA, Justification of Estimates for Appropriations Committees, FY2019, Rockville, MD and HRSA, Health Workforce, "Teaching Health Centers Graduate Medical Education Program: Academic Year 2016-2017," https://bhw.hrsa.gov/sites/default/files/bhw/health-workforce-analysis/program-highlights/THCGME-program-2017.pdf. |
| 129. |
The Uniformed Services University of Health Sciences (USUHS) is a federal health professions academy administered by the DOD. The statutory authority for USUHS is found in chapter 104 of title 10, United States Code. |
| 130. |
Confidential communication from DOD officials, 2018. |
| 131. |
See PDF pages 129-130 at http://comptroller.defense.gov/Portals/45/Documents/defbudget/fy2016/budget_justification/pdfs/09_Defense_Health_Program/DHP_PB16_Vol_I-II.pdf. |
| 132. |
GAO Health Care Workforce Report. |
| 133. |
Confidential communication from DOD officials, 2018. |
| 134. |
Ibid. |
| 135. |
GAO Health Workforce Planning Report. |
| 136. |
GAO Health Workforce Planning Report. GAO's critiques also included nonphysician training through Medicare and Medicaid GME payment programs. |
| 137. |
GAO 2018 GME Information. |
| 138. |
COGME, Towards the Development of a National Strategic Plan for Graduate Medical Education, 23rd Report, Rockville, MD, April 2017. |
| 139. |
For example, the need for more data was among the recommendations in the 2014 IOM GME Report. |
| 140. |
GAO 2018 GME Information. |
| 141. |
Ibid. |
| 142. |
Marsha Regenstein et al., "Comprehensive Revenue and Expense Data Collection Methodology for Teaching Health Centers: A Model for Accountable Graduate Medical Education Financing," Journal of Graduate Medical Education, vol. 10, no. 4 (April 2018), pp. 157-164. |
| 143. |
Ibid., and Barbara O. Wynn, "Is the Teaching Health Center Graduate Medical Education Program a Model for GME Reform?" Journal of Graduate Medical Education, vol. 10, no. 2 (April 2018), pp. 165-167. |
| 144. |
HRSA, "Proposed Standards for the Children's Hospitals Graduate Medical Education Payment Program's Quality Bonus System," 83 Federal Register 29796-29798, June 26, 2018. |
| 145. |
National Academy of Medicine, Graduate Medical Education Outcomes and Metrics: Proceedings of a Workshop, Washington, DC, March 27, 2018. |
| 146. |
David A. Asch et al., "Evaluating Obstetrical Residency Programs Using Patient Outcomes," JAMA, vol. 302, no. 12 (September 23, 2009), pp. 1277-1283, and Candice Chen et al., "Spending Patterns in Region of Residency Training and Subsequent Expenditures for Care Provided by Practicing Physicians for Medicare Beneficiaries," JAMA, vol. 312, no. 22 (December 10, 2014), pp. 2385-2393. |
| 147. |
MedPAC conducted these analyses, which have since been used to recommend that IME payments be reduced with savings used for other needs either within GME or for overall deficit reduction. |
| 148. |
See National Commission on Fiscal Responsibility and Reform, "The Moment of Truth," December, 2010, https://www.fiscalcommission.gov/news/; see recommendation 3.35. |
| 149. |
For example, CBO included this proposal in its "Options for Reducing the Deficit: 209-2028," https://files.constantcontact.com/a3c45cb9201/f890eaf6-b16d-4813-ace4-75b2e3c80b16.pdf, pp. 86-88. |
| 150. |
The President's budget for FY2019 proposes to consolidate and reduce the size of federal support for GME over time. Specifically, the proposal would combine Medicare, Medicaid, and CHGME GME spending in 2019 and redistribute these funds to hospitals based on the number of residents that the hospital trained (up to a hospital's existing Medicare or CHGME cap) and the proportion of the hospital's patients who are Medicare or Medicaid beneficiaries. This amount would increase for inflation over time, less than 1% annually. See HRSA, Justification of Estimates for Appropriations Committees, FY2019, Rockville, MD, p. 149. |
| 151. |
For example, in the 115th Congress, legislation has been introduced that would expand GME support (e.g., H.R. 1667, H.R. 2267, S. 1301). |
| 152. |
See discussion in "GME Policy and Health Workforce Data" section. |
| 153. |
Edward Salsberg et al., "U.S. Residency Training Before and After the 1997 Balanced Budget Act," Journal of the American Medical Association, vol. 300, no. 10 (September 10, 2008), pp. 1174-1180 and Barbara O. Wynn, "Is the Teaching Health Center Graduate Medical Education Program a Model for GME Reform?" Journal of Graduate Medical Education, vol. 10, no. 2 (April 2018), pp. 165-167. |
| 154. |
A 2013 report by MedPAC examined this issue; see MedPAC, "Does It Cost More to Train Residents or to Replace Them?" September 2013, www.medpac.gov/documents/contractor-reports/sept13_residents_gme_contractor.pdf?sfvrsn=0. |
| 155. |
Jose A. Perez et al., "Comparison of Direct Patient Care Costs and Quality Outcomes of the Teaching and Non-Teaching Hospitalist Service at a Large Academic Medical Center," Academic Medicine, vol. 93, no. 3 (February 2018), pp. 491-497 and Michael C. Iannuzzi et al., "Comparing Hospitalist-Resident to Hospitalist-Midlevel Practitioner Team Performance on Length of Stay and Direct Patient Care Cost," Journal of Graduate Medical Education, vol. 7, no. 1 (March 2015), pp. 65-69. In addition, see MEDPAC's June 2009 Report and June 2010 Report to Congress, and 2014 IOM GME Report. All of these reports note the possibility that, in some cases, residents (particularly those in later years of training) may generate revenue for the hospital where they are training. Other research has also found that hospitals using residents may have lower costs per case with similar outcomes when compared to similar cases that did not have residents participating in their care. |
| 156. |
For example, the ACA redistributed Medicare-funded residency slots and required hospitals to use some of these slots to training primary care physicians. See CRS Report R41278, Public Health, Workforce, Quality, and Related Provisions in ACA: Summary and Timeline. |
| 157. |
Stephen Petterson, Matthew Burke, Robert Phillips, et al., "Accounting for Graduate Medical Education Production of Primary Care Physicians and General Surgeons: Timing of Measurement Matters," Academic Medicine, vol. 86, no. 5 (May 2011). |
| 158. |
For example, one study found that Medicare's DGME per resident amounts were "76% of actual fiscal year 2011 per-resident costs," see MedPAC, "Does It Cost More to Train Residents or to Replace Them?" September 2013, www.medpac.gov/documents/contractor-reports/sept13_residents_gme_contractor.pdf?sfvrsn=0. |
| 159. |
GAO 2018 GME Information. |
| 160. |
CRS Report R41278, Public Health, Workforce, Quality, and Related Provisions in ACA: Summary and Timeline. |
| 161. |
GAO Health Workforce Planning Report, pp. 20. |
| 162. |
GAO, Locations and Types of Graduate Training Were Largely Unchanged, and Federal Efforts May Not Be Sufficient to Meet Needs, 17-411, May 25, 2017. |
| 163. |
For example, the 2014 IOM GME Report. |
| 164. |
In its 2018 report, GAO specifically noted that because Medicaid is administered by states CMS has little program information. GAO 2018 GME Information. |
