The Veterans Choice Program (VCP): Program Implementation
Authorized under Section 101 of the Veterans Access, Choice, and Accountability Act of 2014 (VACAA), the Veterans Choice Program (VCP) is a temporary program that enables eligible veterans to receive medical care in the community. Since the program was first established by VACAA, it has been amended and funded several times. More recently, P.L. 115-26 eliminated the August 7, 2017, expiration date for the VCP and allowed the program to continue until the initial $10 billion deposited in the Veterans Choice Fund (VCF) was expended. P.L. 115-46 authorized and appropriated an additional $2.1 billion to continue the VCP until funds were expended, and when these funds were also nearing their end, Division D of P.L. 115-96 appropriated an additional $2.1 billion to continue the VCP until funds were expended. Lastly, Section 510 of the VA MISSION Act (P.L. 115-182), signed into law on June 6, 2018, authorized and appropriated $5.2 billion for VCP without fiscal year limitation, and Section 143 of this same act imposed a sunset date that is one year after the date of enactment (June 6, 2018) of the VA MISSION Act (i.e., June 6, 2019). Title 101 of the VA MISSION Act also authorized a permanent program known as the Veterans Community Care Program (VCCP), which is to replace VCP when VCCP is established by the Department of Veterans Affairs (VA) around June 2019 (when regulations are published by the VA no later than one year after the date of enactment [June 6, 2018] of the VA MISSION Act; that is, June 6, 2019, or when the VA determines that 75% of the amounts deposited in the VCF have been exhausted).
Eligibility and Choice of Care
Veterans must be enrolled in the VA health care system to request health services under the VCP. A veteran may request a VA community care consult/referral, or his or her VA provider may submit a VA community care consult/referral to the VA Care Coordination staff within the VA.
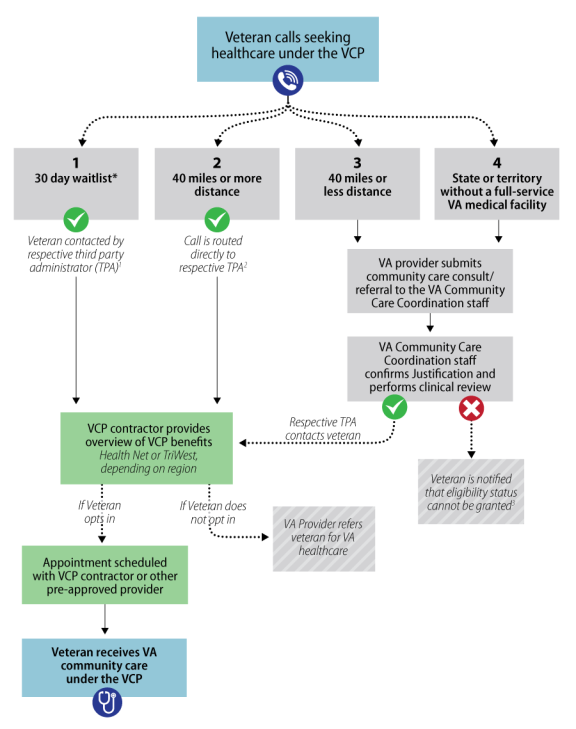
Veterans may become eligible for the VCP in one of four ways. First, a veteran is informed by a local VA medical facility that an appointment cannot be scheduled within 30 days of the clinically determined date requested by his or her VA doctor or within 30 days of the date requested by the veteran (this category also includes care not offered at a veteran’s primary VA facility and a referral cannot be made to another VA medical facility or other federal facility). Second, the veteran lives 40 miles or more from a VA medical facility that has a full-time primary care physician. Third, the veteran lives 40 miles or less (not residing in Guam, America Samoa, or the Republic of the Philippines) and either travels by air, boat, or ferry to seek care from his or her local facility or incurs a traveling burden of a medical condition, geographic challenge, or an environmental factor. Fourth, the veteran resides 20 miles or more from a VA medical facility located in Alaska, Hawaii, New Hampshire (excluding those who live 20 miles from the White River Junction VAMC), or a U.S. territory, with the exception of Puerto Rico.
Once found eligible for care through the VCP, veterans may choose to receive care from a VA provider or from an eligible VA community care provider (VCP provider). VCP providers are federally qualified health centers, Department of Defense (DOD) facilities, or Indian Health Service facilities, and hospitals, physicians, and nonphysician practitioners or entities participating in the Medicare or Medicaid program, among others. A veteran has the choice to switch between a VA provider and VCP provider at any time.
Program Administration and Provider Participation
The VCP was administered by two third-party administrators (TPAs): Health Net and TriWest. At the end of September 2018, the VA has announced that it would end its contract with Health Net as a TPA because of low patient volume, customer service issues, and late payments to community providers in its network. TriWest would continue to be a TPA for the areas they manage. Generally, a TPA manages veterans’ appointments, counseling services, card distributions, and a call center. The TPA contracts directly with the VA. Then, the TPA contracts with eligible non-VA community care providers interested in participating in the VCP.
Payments
Generally, a veteran’s out-of-pocket costs under the VCP are equal to VHA out-of-pocket costs. Veterans do not pay any copayments at the time of their medical appointments. Copayment rates are determined by the VA after services are furnished. Enactment of P.L. 115-26 on April 19, 2017, allowed VA to become the primary payer when certain veterans with other health insurance (OHI) receive care for nonservice-connected conditions under VCP—veterans would not have to pay a copayment under their OHI anymore. The VA would coordinate with a veteran’s OHI and bill for any copayments that the veteran would be responsible for similar to what they would have paid had they received care within a VA medical facility. Participating community providers are reimbursed by their respective TPA, and VA pays the TPAs on an aggregated basis, known as bulk payments.
The Veterans Choice Program (VCP): Program Implementation
Jump to Main Text of Report
Contents
- Introduction
- Scope and Limitations
- Medical Services Under VCP
- Eligibility
- Choice of Care
- VCP Providers
- Program Administration
- Third-Party Administrators (TPAs)
- End of Contract with Health Net
- Community Care Provider Participation
- Consults/Referral Processes
- Unusual or Excessive Burden Determination
- Authorization of Care and an Episode of Care
- Appointment Scheduling
- Medication Process
- Processing Medical Claims
- Medical Services Not Previously Authorized
- Payments
- Veterans' Out-of-Pocket Costs
- Cost Shares for Veterans with Other Health Insurance (OHI)
- Provider Payment Methodologies
Figures
- Figure 1. Eligibility Process to Access Care through the Veterans Choice Program (VCP)
- Figure 2. VCP Regions Covered by Third-Party Administrators
- Figure 3. Coordination and Billing for Nonservice-Connected Care for Veterans with Other Health Insurance (OHI)
- Figure A-1. High-Level Work Flow of Obtaining Care Through VCP
- Figure B-1. VA Fact Sheet for Veterans
- Figure B-2. VA Fact Sheet for VCP Providers
- Figure B-3. VA Fact Sheet for VA Staff
Tables
Summary
Authorized under Section 101 of the Veterans Access, Choice, and Accountability Act of 2014 (VACAA), the Veterans Choice Program (VCP) is a temporary program that enables eligible veterans to receive medical care in the community. Since the program was first established by VACAA, it has been amended and funded several times. More recently, P.L. 115-26 eliminated the August 7, 2017, expiration date for the VCP and allowed the program to continue until the initial $10 billion deposited in the Veterans Choice Fund (VCF) was expended. P.L. 115-46 authorized and appropriated an additional $2.1 billion to continue the VCP until funds were expended, and when these funds were also nearing their end, Division D of P.L. 115-96 appropriated an additional $2.1 billion to continue the VCP until funds were expended. Lastly, Section 510 of the VA MISSION Act (P.L. 115-182), signed into law on June 6, 2018, authorized and appropriated $5.2 billion for VCP without fiscal year limitation, and Section 143 of this same act imposed a sunset date that is one year after the date of enactment (June 6, 2018) of the VA MISSION Act (i.e., June 6, 2019). Title 101 of the VA MISSION Act also authorized a permanent program known as the Veterans Community Care Program (VCCP), which is to replace VCP when VCCP is established by the Department of Veterans Affairs (VA) around June 2019 (when regulations are published by the VA no later than one year after the date of enactment [June 6, 2018] of the VA MISSION Act; that is, June 6, 2019, or when the VA determines that 75% of the amounts deposited in the VCF have been exhausted).
Eligibility and Choice of Care
Veterans must be enrolled in the VA health care system to request health services under the VCP. A veteran may request a VA community care consult/referral, or his or her VA provider may submit a VA community care consult/referral to the VA Care Coordination staff within the VA.
Veterans may become eligible for the VCP in one of four ways. First, a veteran is informed by a local VA medical facility that an appointment cannot be scheduled within 30 days of the clinically determined date requested by his or her VA doctor or within 30 days of the date requested by the veteran (this category also includes care not offered at a veteran's primary VA facility and a referral cannot be made to another VA medical facility or other federal facility). Second, the veteran lives 40 miles or more from a VA medical facility that has a full-time primary care physician. Third, the veteran lives 40 miles or less (not residing in Guam, America Samoa, or the Republic of the Philippines) and either travels by air, boat, or ferry to seek care from his or her local facility or incurs a traveling burden of a medical condition, geographic challenge, or an environmental factor. Fourth, the veteran resides 20 miles or more from a VA medical facility located in Alaska, Hawaii, New Hampshire (excluding those who live 20 miles from the White River Junction VAMC), or a U.S. territory, with the exception of Puerto Rico.
Once found eligible for care through the VCP, veterans may choose to receive care from a VA provider or from an eligible VA community care provider (VCP provider). VCP providers are federally qualified health centers, Department of Defense (DOD) facilities, or Indian Health Service facilities, and hospitals, physicians, and nonphysician practitioners or entities participating in the Medicare or Medicaid program, among others. A veteran has the choice to switch between a VA provider and VCP provider at any time.
Program Administration and Provider Participation
The VCP was administered by two third-party administrators (TPAs): Health Net and TriWest. At the end of September 2018, the VA has announced that it would end its contract with Health Net as a TPA because of low patient volume, customer service issues, and late payments to community providers in its network. TriWest would continue to be a TPA for the areas they manage. Generally, a TPA manages veterans' appointments, counseling services, card distributions, and a call center. The TPA contracts directly with the VA. Then, the TPA contracts with eligible non-VA community care providers interested in participating in the VCP.
Payments
Generally, a veteran's out-of-pocket costs under the VCP are equal to VHA out-of-pocket costs. Veterans do not pay any copayments at the time of their medical appointments. Copayment rates are determined by the VA after services are furnished. Enactment of P.L. 115-26 on April 19, 2017, allowed VA to become the primary payer when certain veterans with other health insurance (OHI) receive care for nonservice-connected conditions under VCP—veterans would not have to pay a copayment under their OHI anymore. The VA would coordinate with a veteran's OHI and bill for any copayments that the veteran would be responsible for similar to what they would have paid had they received care within a VA medical facility. Participating community providers are reimbursed by their respective TPA, and VA pays the TPAs on an aggregated basis, known as bulk payments.
Introduction
In response to concerns about access to medical care at many Department of Veterans Affairs (VA) hospitals and clinics across the country in spring 2014,1 Congress passed the Veterans Access, Choice, and Accountability Act of 2014 (VACAA, P.L. 113-146, as amended). On August 7, 2014, President Obama signed the bill into law.2 Since the VACAA was enacted, Congress has amended the act several times: P.L. 113-175, P.L. 113-235, P.L. 114-19, P.L. 114-41, P.L. 115-26, P.L. 115-46, P.L. 115-96, and P.L. 115-182. In addition, the VA has issued implementation regulations and guidance on several occasions in response to the changes to VACAA and challenges encountered during implementation of the law. Table 1 provides major highlights pertaining to the Veterans Choice Program (VCP)―a new, temporary program authorized by Section 101 of the VACAA that allows eligible veterans to receive medical care in the community.
|
Date |
Action |
|
August 7, 2014 |
The Veterans Access, Choice, and Accountability Act of 2014 (P.L. 113-146) signed into law. The Secretary of Veterans Affairs is required to publish regulations in the Federal Register for the implementation of Veterans Choice Program (VCP) no later than November 5, 2014. |
|
September 26, 2014 |
The Department of Veterans Affairs Expiring Authorities Act of 2014 (P.L. 113-175) was signed into law. The act makes several technical amendments to the Veterans Access, Choice, and Accountability Act of 2014 (P.L. 113-146). |
|
November 5, 2014 |
The Department of Veterans Affairs issues interim final rules implementing the Veterans Choice Program (VCP). VA begins mailing out a Choice Card to every enrolled veteran and every separating servicemember. |
|
December 16, 2014 |
The Consolidated and Further Continuing Appropriations Act, 2015 (P.L. 113-235) is signed into law. The act made several technical amendments allowing the VA to reimburse providers in the state of Alaska, under the VA Alaska Fee Schedule, and in states with an "All-Payer Model" agreement, VA was allowed to calculate Medicare payments based on payment rates under such "All-Payer Model" agreements. |
|
April 24, 2015 |
The Department of Veterans Affairs issues interim final rules modifying how VA measures the distance from a veteran's residence to the nearest VA medical facility. This modification considered the distance the veteran must drive to the nearest VA medical facility from the veteran's residence, rather than the straight-line or geodesic distance to the VA facility. |
|
May 12, 2015 |
Department of Veterans Affairs issues memorandum to Veterans Integrated Service Network (VISN) Directors on VA Care in the Community (Non-VA Purchased Care) and use of the Veterans Choice Program. The memorandum outlines that effective June 8, 2015, a specific hierarchy of care must be used when the veteran's primary VA medical facility cannot readily provide needed care to a veteran, either because the care is unavailable at the facility or because the facility cannot meet VHA's wait time criteria. |
|
May 22, 2015 |
The Construction Authorization and Choice Improvement Act was signed into law (P.L. 114-19) and amended the 40 miles eligibility criteria for the Veterans Choice Program (VCP) to clarify that the 40 miles is calculated based on distance traveled (driving distance) rather than the previous straight-line or geodesic distance standard, and authorized VA to determine if there is an unusual or excessive burden in traveling to a VA medical facility. |
|
July 31, 2015 |
The Surface Transportation and Veterans Health Care Choice Improvement Act (P.L. 114-41) is signed into law. Among other things, the act allowed all enrolled veterans to be eligible for the Veterans Choice Program (amended the August 1, 2014, enrollment date restriction), defined the nearest VA medical facility as a Community Based Outpatient Clinic (CBOC) with no full time primary care physician, removed the 60-day limitation on an episode of care, included clinically indicated date as a wait time eligibility criteria, and expanded provider eligibility. |
|
October 1, 2015 |
Department of Veterans Affairs issues memorandum to Veterans Integrated Service Network (VISN) Directors on VA Care in the Community (Non-VA Purchased Care) and use of the Veterans Choice Program that modifies the May 12, 2015, memorandum. The memorandum provides guidance on the hierarchy of care in the Veterans Choice Program (VCP). This allows VA medical facilities to refer the veteran to VCP for care not available at the veteran's primary VA medical facility and for which a referral pattern does not exist to another VA medical facility or other federal facility. |
|
October 29, 2015 |
The Department of Veterans Affairs (VA) publishes final rules based on interim final rules published on November 5, 2014, and on April 24, 2015. These rules do not incorporate amendments to the Veterans Choice Program (VCP) made by the Surface Transportation and Veterans Health Care Choice Improvement Act (P.L. 114-41). |
|
December 1, 2015 |
The Department of Veterans Affairs (VA) publishes interim final rules revising previous VA regulations implementing the Veterans Choice Program (VCP) based on amendments made by the Construction Authorization and Choice Improvement Act was signed into law (P.L. 114-19) and the Surface Transportation and Veterans Health Care Choice Improvement Act (P.L. 114-41). |
|
April 19, 2017 |
P.L. 115-26 (unofficially referred to as the Veterans Choice Program Improvement Act) eliminates the August 7, 2017, sunset date of the Veterans Choice Program (VCP) and authorizes the program to continue until all the funds in the Veterans Choice Fund established by Section 802 of the Veterans Access, Choice, and Accountability Act of 2014 are expended. Furthermore, P.L. 115-26 authorized the Department of Veterans Affairs (VA) to become the primary payer for veterans with other health insurance (OHI) for care or services related to a nonservice-connected disability for which the veteran is entitled to care under the veteran's OHI. The VA would coordinate with the veteran's OHI and bill for any copayments that the veteran would be responsible for similar to what they would have paid had they received medical care or services within a VA medical facility. |
|
August 12, 2017 |
The VA Choice and Quality Employment Act of 2017 (P.L. 115-46) authorized and appropriated $2.1 billion for the Veterans Choice Fund (established by Section 802 of the Veterans Access, Choice, and Accountability Act of 2014). Funds would remain available until expended. |
|
December 20, 2017 |
The VA publishes a notice in the Federal Register indicating that all amounts deposited in the Veterans Choice Fund would be exhausted sometime between January 2, 2018, and January 16, 2018. |
|
December 22, 2017 |
The President signed into law P.L. 115-96 (an act to amend the Homeland Security Act of 2002 to require the Secretary of Homeland Security to issue Department of Homeland Security-wide guidance and develop training programs as part of the Department of Homeland Security Blue Campaign, and for other purposes). Division D of P.L. 115-96 appropriated an additional $2.1 billion for the Veterans Choice Fund. Funds would remain available until expended. |
|
June 6, 2018 |
VA Maintaining Internal Systems and Strengthening Integrated Outside Networks Act of 2018 (VA MISSION Act of 2018) is signed into law (P.L. 115-182). Section 143 of the VA MISSION Act of 2018 establishes a sunset date for the VCP, which is one year after the date of enactment of the VA MISSION Act, i.e. June 6, 2019. Additionally, Section 510 of this act provides $5.2 billion in mandatory funds for the Veterans Choice Fund that would remain available without fiscal year limitations. |
On June 6, 2018, President Donald Trump signed the John S. McCain III, Daniel K. Akaka, and Samuel R. Johnson VA Maintaining Internal Systems and Strengthening Integrated Networks Act of 2018 (the VA MISSION Act of 2018) into law (P.L. 115-182). Section 101 of this act established a new permanent Veterans Community Care Program (VCCP) that would replace VCP. This new program is expected to be operational around June 6, 2019. (The MISSION Act of 2018 stipulates that VCCP must be effective when the VA determines that 75% of the amounts deposited in the Veterans Choice Fund [VCF] have been exhausted, or when regulations are published by the VA, which is no later than one year after the date of enactment of the VA MISSION Act—June 6, 2019.)
This report provides details on how the VCP is being implemented. It is meant to provide insight into the execution of the current VCP program that is still functioning until the new VCCP program becomes operational sometime in June 2019.
Scope and Limitations
Information contained in this report is drawn from regulations published in the Federal Register, conference calls, numerous meetings with VHA staff, and briefing materials and other information provided by the VA Office of Congressional and Legislative Affairs (which may not be publicly available). This report does not discuss the new VCCP program established by Section 101 of the VA MISSION Act of 2018.
Medical Services Under VCP
Once an eligible veteran is authorized to receive necessary treatment, including follow-up appointments and ancillary and specialty medical services, under the VCP, a veteran may receive similar services that are offered through their personalized standard medical benefits package at a VA facility. VA's standard medical benefits package includes (but is not limited to) inpatient and outpatient medical, surgical, and mental health care; pharmaceuticals; pregnancy and delivery services; dental care; and durable medical equipment, and prosthetic devices, among other things.3 Currently, 81 categories of medical services and procedures are authorized to be provided under VCP.4 However, institutional long-term care and emergency care in non-VA facilities are excluded from the VCP. "It is important to note that the VCP does not provide guaranteed health care coverage or an unlimited medical benefit."5 These services are authorized and provided under separate statutory authorities outside the scope of VCP.
Eligibility
Generally, all veterans have to be enrolled in the VA health care system6 to receive care under the VCP. Once this initial criterion is met, a qualified veteran may choose to receive care through VCP. Veterans may become eligible for care under the VCP through one of four different pathways:7
- 30-day wait list (Wait-Time Eligible): A veteran is eligible for care through the VCP when he or she is informed, by a local VA medical facility, that an appointment cannot be scheduled
- within 30 days of the clinically determined date of when the veteran's provider determines that he or she needs to be seen (this category also includes care not offered at the veteran's primary VA medical facility and a referral cannot be made to another VA medical facility or federal facility),8 or
- within 30 days of the date of when the veteran wishes to be seen.
- 40 miles or more distance (Mileage Eligible): A veteran is eligible for care through the VCP when he or she lives 40 miles or more from a VA medical facility that has a full-time primary care physician.
- 40 miles or less distance (Mileage Eligible): A veteran is eligible for care through the VCP when he or she resides in a location, other than one in Guam, American Samoa, or the Republic of the Philippines, and
- travels by air, boat, or ferry in order to seek care from his or her local VA facility; or
- incurs a traveling burden9 based on environmental factors, geographic challenges, or a medical condition.10
- State or territory without a full-service VA medical facility: A veteran is eligible for care through the VCP when his or her residence is more than 20 miles from a VA medical facility and located in either
- Alaska,
- Hawaii,
- New Hampshire (excluding veterans who live 20 miles from the White River Junction VAMC), or
- U.S. territory (excluding Puerto Rico).
Table 2 provides a breakdown of the unique number of veterans utilizing the VCP, by eligibility category, from November 2014 through August 28, 2018, unless otherwise noted.
|
Wait-Time Eligible (VACAA, §101(b)(2) (A)) |
Choice First (June 2015- August 28, 2018)a |
Mileage Eligible (VACAA, §101(b)(2) (B)) |
Resides in a State Without VA Medical Facility (VACAA, 101(b)(2)(C)) |
Unusual/ |
|
|
Unique Veterans |
908,884 |
1,213,869 |
206,580 |
56,183 |
1,431 |
Source: Data provided by the Department of Veterans Affairs, using self-reported weekly data by the Third-Party Administrators, and has not been validated. The data fluctuate from the monthly validated reports, and they cannot be reconciled. However, according to the department, these are the best data currently available.
Notes: The total number of unique veterans cannot be added across rows, as a veteran may be counted in more than one eligibility category. Unique veterans are counted using the social security number per eligibility category and have completed at least one appointment under that eligibility category; excludes any return authorizations.
a. Effective June 2015, the VA provided guidance on the hierarchy of care in the Veterans Choice Program (VCP). This allows VA medical facilities to refer the veteran to VCP for care not available at the veteran's primary VA medical facility and for which a referral pattern does not exist to another VA medical facility or other federal facility. This initiative is known as "Choice First."
A veteran who believes that he or she meets one of the eligibility criteria to receive care through the VCP is to have his or her eligibility status confirmed by local VA staff. A high-level overview of the eligibility process to access care through the VCP is illustrated in Figure 1. Local VA facility staff members are to review clinical and administrative records of the veteran to determine the appropriate medical benefits package and clinical criterion. Confirmation of the veteran's eligibility status is generally determined within 10 business days from when the request for confirmation was submitted. Veterans who are found ineligible to participate in the VCP are to be given instructions, in their notification letters, on how to appeal the VA's decision.11 Also see Appendix A for a detailed high-level workflow of how care is obtained through VCP.
Choice of Care
Eligible veterans have two options for receiving health care services under the Veterans Choice Program (VCP). First, veterans may choose to receive their medical care from a VA provider. A veteran who chooses this option is to receive an appointment with a VA provider. The veteran may be offered a VA appointment that is more than 30 days out or at a facility that is more than 40 miles from the veteran's residence.12 If an offered appointment does not accommodate the veteran's clinical needs, the local VA staff may place the veteran on an electronic waiting list until an alternate appointment becomes available. At any time, the veteran (based on the availability of clinical appointments) may choose to receive his or her medical services from a VA community care provider.
|
Two Options for Choosing Care under the Veterans Choice Program (VCP) Based on the availability of appointments,
|
The second option allows veterans to receive health care services from a VA community care provider (VCP provider) who accepts eligible VCP veterans. Veterans who choose this option are to have their names and medical authorization information sent to a VCP provider of their choice.13 At any time, veterans (based on the availability of clinical appointments) may choose to receive their medical services from a VA provider.
VCP Providers
Under the VCP, several entities and providers are eligible to provide care and services. These include, among others, federally qualified health centers, Department of Defense (DOD) medical facilities, Indian Health Service outpatient health facilities or facilities operated by a tribe or tribal organization, hospitals, physicians, and nonphysician practitioners or entities participating in the Medicare or Medicaid program, an Aging and Disability Resource Center, an area agency on aging, or a state agency or a center for independent living. VA employees are excluded from providing care or services under VCP, unless the provider is an employee of VA, and is not acting within the scope of such employment while providing hospital care or medical services through the VCP.14 Generally, VCP providers "must maintain at least the same or similar credentials and licenses as those required of VA's health care providers."15
Program Administration
The Veterans Choice Program (VCP) is not a health insurance plan for veterans. Under the VCP, veterans are given the option of receiving care in their local communities instead of waiting for a VA appointment and/or enduring traveling burdens to reach a VA facility.16
All veterans who are enrolled in the VA health care system are to be mailed a VCP card. The card lists relevant information about the VCP. Many veterans have attempted to use the VCP card as an insurance card. The VCP card may not be used to pay for medical services performed outside of or within the VA. Specifically, the VCP card does not
- replace veterans' identification cards,
- guarantee eligibility under the VCP,17 or
- provide health insurance-like benefits (i.e., the VCP, like all VA health care, is not health insurance).
Third-Party Administrators (TPAs)
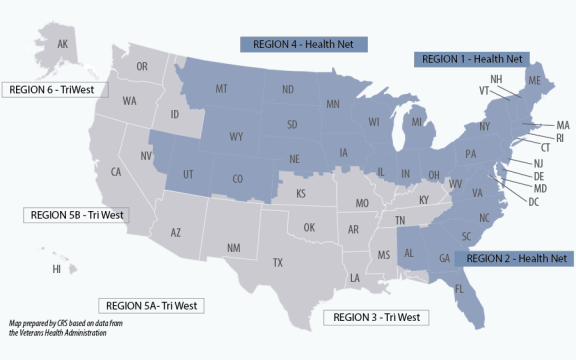
In September 2013, the VA awarded contracts to Health Net18 and TriWest19 to expand veterans' access to non-VA health care in the communities, under the Patient-Centered Community Care (PC3) initiative.20 Later, in November 2014, the VA modified those contracts to include support services under the Veterans Access, Choice, and Accountability Act of 2014 (VACAA, or the Choice Act). Under the Veterans Choice Program (VCP), Health Net and TriWest manage the appointments, counseling services, card distributions, and a call center.21 They also oversee VCP providers, medical services reporting and billing processes, and the coordination of care with private health insurers. As illustrated in Figure 2, Health Net covers Regions 1, 2, and 4, and TriWest covers Regions 3, 5A, 5B, and 6.
End of Contract with Health Net
In March 2018, the VA announced that the VCP contract with Health Net would end by September 30, 2018.22 Low volume of patients, customer service issues, and delayed payments to community providers were potentially some of the reasons for this decision.23 The contract with TriWest would continue. The VA has issued guidance to veteran patients, community providers, and local VA medical center staff regarding next steps after the contract with Health Net ends in September 2018. These documents have been reproduced in their entirety in Appendix B. Activities previously undertaken by Health Net, such as VCP authorizations, care coordination, and billing and payments, will now be managed directly between local VA medical centers and community care providers.
 |
|
Source: Map prepared by CRS based on data from the Veterans Health Administration. Notes: Beginning September 30, 2018, Health Net would no longer administer the contracted network regions shown above, and would not perform certain administrative tasks for the VA. These activities, including VCP authorizations, care coordination, and billing and payments, will be managed directly between the VA and community care providers. |
Community Care Provider Participation24
Eligible non-VA community care providers may become VCP providers. Providers who are interested in participating in the VCP may do so either through the Patient Centered Community Care (PC3) network or the Choice network. Community providers who are under the Choice network may only render authorized services to VCP-eligible veterans. Under the PC3 network, all veterans who are eligible for VA community care may be seen.25 The reason is that there are two different statutory authorities for care delivered through VCP and PC3. Interested providers are required to contact TriWest to determine whether they qualify as a VA community care provider.26 To qualify, providers must meet the following criteria:
- Have a full, current, and unrestricted state license and the same/similar VA credentials.
- Not be named on the Centers for Medicare and Medicaid Services (CMS) exclusionary list.27
- Meet all Medicare Conditions of Participation (CoPs) and Conditions for Coverage (CfCs).28
- Accept Medicare or Medicaid rates.
- Provide resources (services, facilities, and providers) that are in compliance with applicable federal and state regulatory requirements.
- Submit all medical records of rendered services to veterans to the TPA for inclusion in veterans' VA electronic medical records.
After determining that a provider is eligible for participation, he or she may enroll (with TriWest) as a VCP provider. At this time, the VA community care provider and respective third-party administrator (TPA) are to establish an agreed-upon reimbursement amount for rendered services to veterans. When TriWest is unable to coordinate the delivery of health care services to veterans, local VA Medical Centers (VAMCs) may enter into VCP Provider Agreements with eligible VA community providers through the VAMCs' Community Care Departments.29
Consults/Referral Processes30
Consults and referrals, known as the VA community care consults/referrals, are initiated in two different manners.31 First, a VA physician may submit a VA community care consult/referral (through the Computerized Patient Record System [CPRS])32 on behalf of a veteran when there is a clinical need for the veteran to receive timely medical services. Second, a veteran may request a VA community care consult/referral (from his or her VA provider or local VA staff) in order to receive a medical service that is also timely. Regardless of how the consult/referral is initiated, all VA community care consults/referrals are to be processed by the VA Community Care Coordination staff within the VA. VA community care consults/referrals are processed based on whether the veteran requires emergent or urgent care. For urgent VA community care consults/referrals, VA providers are to coordinate the veteran's care directly with the VA Community Care Coordination staff.
When a veteran's request for a VA community care consult/referral cannot be approved, the veteran's local VA facility staff are to notify the veteran. On behalf of the veteran, his or her VA provider is to continue coordinating the veteran's medical services within the VA. The veteran's provider might also explore other existing community care options offered by the Veterans Health Administration (VHA).
After a veteran's request is approved or the VA community care consult/referral is submitted by the veteran's provider, the VA Community Care Coordination staff are to confirm the veteran's eligibility status. A veteran may decline enrollment into the VCP. When a veteran declines enrollment, his or her respective third-party administrator (TPA) is to document the veteran's reason for opting out of the program. Then, on behalf of the veteran, his or her VA provider is to continue coordinating the veteran's medical services within the VA. The veteran's provider might also explore other existing community care options offered by the VHA.
If a veteran is found eligible to access care through the VCP, the VA Community Care Coordination staff is to then electronically upload the veteran's VA community care consult/referral and pertinent medical documentation in the Contractor Portal, which is visible to TriWest. Once TriWest receives the documentation, the respective TPA is to contact the veteran. During this contact, the eligible veteran is to be provided with an overview of VCP benefits and asked to confirm his or her choice to receive medical services under the VCP.
If a veteran reiterates his or her choice to receive medical care under the VCP, the veteran may select his or her VA community care provider and coordinate with a TPA to schedule an appointment. In addition, the veteran is to be asked to provide other health insurance information, if applicable, and is made aware of possible copayments and deductibles. A veteran with a clinical need for a service-connected and/or special authority condition33 (SC/SA) is to have his or her screening information reviewed by Revenue Utilization Review (R-UR)34 nurses. The veteran's appointment is then to be entered in the Contractor Portal so that it can be viewed by the VA Community Care Coordination staff. Daily, the VA Community Care Coordination staff is to check the Contractor Portal for appointment statuses and other updates. After the appointment is scheduled, the VA Community Care Coordination staff are to enter the appointment information into the Appointment Management system (within the VA) and update the veteran's status to "scheduled."
Unusual or Excessive Burden Determination35
Along with the environmental factors, geographic challenges, and medical conditions, veterans are assessed by
- the nature or simplicity of the hospital care or medical services the veteran requires,
- how frequently the veteran needs hospital care or medical services, and
- the need for an attendant for a clinical service.36
Authorization of Care and an Episode of Care
Prior to delivering medical services to veterans under the Veterans Choice Program (VCP), such services are to be authorized by the VA.37 If a veteran requires services beyond those authorized, his or her VCP provider may request another authorization. The delivery and usage of unauthorized medical services could result in nonreimbursement. Over 5.9 million authorizations have been made under the VCP. These authorizations of care, shown in Table 3, were authorized from November 5, 2014, to August 28, 2018, unless otherwise noted.
Table 3. Authorizations of Care for the Veterans Choice Program
(Note that one veteran patient could have more than one authorization; data from November 2014 to August 28, 2018)
|
Health Net |
TriWest |
Provider Agreementsa |
Totals |
|
|
Authorizations: Wait-Time Eligibleb |
588,468 |
1,008,505 |
— |
1,596,973 |
|
Authorizations: care is unavailable at the veteran's primary VA medical facility and cannot be referred to another VA facility—"Choice First" (June 2015- August, 28, 2018)c |
900,248 |
1,538,276 |
— |
2,438,524 |
|
Subtotal Unique Authorizations: Wait-Time Eligible |
1,488,716 |
2,546,781 |
— |
4,035,497 |
|
Authorizations: Mileage Eligibleb |
200,169 |
446,241 |
— |
646,410 |
|
Authorizations: Resides in a State without a VA Medical Facilityb |
9,893 |
170,806 |
— |
180,699 |
|
Authorizations: Unusual or Excessive Travel Burden (June 2017-August 28, 2018)b |
796 |
4,876 |
— |
5,672 |
|
Authorizations: Eligibility not categorizedb |
19,796 |
369,559 |
— |
389,355 |
|
Total Authorizations |
1,719,370 |
3,538,263 |
652,080 |
5,909,713d |
Source: Data provided by the Department of Veterans Affairs, using self-reported weekly data by the Third-Party Administrators, and have not been validated except for provider agreement information. The data fluctuate from the monthly validated reports, and they cannot be reconciled. However, according to the department, these are the best data currently available.
a. To receive payment for hospital care or medical services furnished under the VCP, the non-VA hospital care or medical services provider is required to sign an agreement to provide eligible veterans with hospital care and/or medical services authorized by the VA (VA FORM 10-10145) if they are not part of a TPA network.
b. Each authorization for an episode of care under this category is counted only once.
c. Based on the Department of Veterans Affairs, VA Care in the Community (Non-VA Purchased Care) and use of the Veterans Choice Program, Memorandum from Acting Principal Deputy Under Secretary for Health to Veterans Integrated Service Network (VISN) Directors, May 12, 2015, and amended on October 1, 2015, VA categorizes care that is unavailable at the veteran's primary medical facility and that cannot be referred to another VA facility or federal facility as care that would qualify for VCP under the wait-time eligible category.
d. This total includes the 652,080 noncategorized provider agreement authorizations.
The VA defines an episode of care (EOC) as "a necessary course of treatment, including follow-up appointments and ancillary and specialty services, which last no longer than one calendar year from the date of the first appointment with a non-VA health care provider."38 This one-year Choice EOC period of validity begins when the first appointment is scheduled. VA community care providers may request an authorization extension for a veteran's current EOC through the veteran's respective TPA.
Appointment Scheduling
Veterans and VCP providers verify eligibility status before scheduling medical appointments for clinical needs. Appointments are to be scheduled on the basis of clinical appropriateness.39 VCP-eligible veterans are to receive a call from their respective third-party administrator (TPA). The TPAs are to provide veterans with information about the organization and schedule their appointments. Once appointments are scheduled, the contractor is to inform the VA. Emergent or urgent care authorizations are to be done expeditiously (see text box below).
|
Emergent and Urgent Care Determination VA community care consults/referrals are to be prioritized by urgency levels. Urgency levels to deliver care are different under the VCP. Generally, emergent care under the VCP does not mean an emergency medical condition that needs immediate medical attention (emergency treatment furnished by non-VA providers is authorized under separate statutory authorities and not the VCP). Emergent consults/referrals are to be scheduled within five days from the veteran's consultation date with his or her third-party administrator (TPA). Urgent consults/referrals have a timeframe that is within 48 hours. Furthermore, VA providers may bypass the Choice Program process and contact the VA Community Care Coordination staff directly to schedule an urgent appointment with a VCP provider for their veterans. |
After receiving the notification, a veteran's local VA facility staff are to cancel his or her appointment at the VA. Veterans may also choose to schedule their own appointments after receiving an authorization of care under the VCP.40 If veterans choose to do so, they are asked to provide their appointment information to the TPA.
Appointment information that is provided to the TPA is to get uploaded into the Contractor Portal, so that it can be viewed by the VA Community Care Coordination staff. Daily, the VA Community Care Coordination staff are to check the Contractor Portal for veterans' appointment statuses and other updates. After receiving the notification, the veteran's local VA facility staff are to cancel his/her appointment at the VA.
Medication Process
Veterans may have their prescriptions filled at their local VA pharmacies, non-VA pharmacies, and through the Consolidated Mail Outpatient Pharmacy (CMOP). If the VA is unable to fill a medication request within a prescribed timeframe or one that is not within the VA formulary, a non-VA pharmacy may fill the initial 14-day supply (without refills).41 For veterans who require prescriptions for more than 14 days, the VCP prescribing clinician is to have the remaining supply of medication filled at a VA pharmacy. Similar to the provisions of health care services under the VCP, medications filled at non-VA pharmacies will also require prior authorizations from the VA.
The VA is to reimburse veterans for out-of-pocket expenses related to the purchase of medications that treat service-connected conditions. For nonservice-connected conditions, veterans may also be reimbursed for their out-of-pocket expenses, including those with other health insurance plans.42 To be reimbursed, veterans submit a copy of their prescriptions, authorizations, and original receipts to their local VA Community Care Office. The VA also allows non-VA pharmacies to process medication claims on a veteran's behalf.
Processing Medical Claims
Medical claims under the Veterans Choice Program (VCP) are processed through the veteran's respective third-party administrator (TPA). TriWest uploads and manages veterans' medical claims through the Contractor Portal. Through this web portal, the VA Community Care Coordination staff are to retrieve a veteran's documentation of clinical need and upload it in the veteran's medical records.
The VA community care provider is to submit medical claims to a veteran's respective third-party administrator. After TriWest receives the claim, the TPA is to submit it through its web portal. Subsequently, the VA is to retrieve the documentation from the TPA's web portal and upload it in the veteran's medical records. The VA reimburses the TPAs for the care veterans obtain through the VCP, and the TPA then reimburses the community care providers in their networks.43 Since 2016, the VA has processed payments to the TPA on an aggregated basis known as "bulk payments."44
Per Federal authority, VA is the primary and exclusive payer for medical care it authorizes. As such, non-VA medical care providers may not bill the Veteran or any other party for any portion of the care authorized by VA. Federal law also prohibits payment by more than one Federal agency for the same episode of care; subsequently any payments made by the Veteran, Medicare, or any other Federal agency must be refunded to the payer [from the VCP provider] upon acceptance of VA payment.45
Medical Services Not Previously Authorized
Under the VCP, medical claims for unauthorized non-VA health care services may be submitted to the VA for payment consideration. Veterans, VA community care providers, and persons who paid for services on behalf of a veteran are required to submit to the VA the following documentation:
- a standard billing form,46 or an invoice (i.e., Explanation of Benefits [EOB]), and/or receipt of services paid and/or owed;
- an explanation of the circumstance that led to the veteran receiving unauthorized care outside of the VA;
- any statements and/or supporting documentation;47 and
- VA Form-10-583, Claim for Payment of Cost of Unauthorized Medical Services.48
Payments
Veterans' Out-of-Pocket Costs
Veterans who are enrolled in VA health care do not pay premiums,49 deductibles,50 or coinsurances51 for their medical services. However, they may be required to pay a fixed copayment amount (for nonservice-connected disabilities or conditions) as shown below. When veterans receive care at a VA facility, they do not pay copayments at the time of their medical appointments; copayment rates are determined by the VA after services are furnished—based on if the care was for a service-connected or nonservice-connected condition. Therefore, veterans' out-of-pocket costs under the VCP are the same as if they were receiving care and services from a VA provider in a VA facility—if a veteran does not pay any copayments at VA health care facilities, the veteran will not have to pay any copayments under the VCP.52 For example
- A veteran could pay $50 copayments for a specialty care visit and $15 for a primary care visit for a nonservice-connected disability or condition.
- A veteran in Priority Groups 2 thru 8 could pay a copayment between $5 and $11 per 30-day or less supply of medication.53
- All veterans are exempt from paying copayments for services and medications that are related to a service-connected disability or condition.54
Cost Shares for Veterans with Other Health Insurance (OHI)
The VA defines other health insurance (OHI) as commercial insurance. Commercial insurance, often referred to as private insurance, is not funded by federal and state taxes. This type of insurance is offered by companies such as Blue Cross and Blue Shield, Aetna, Cigna, and the Kaiser Foundation. Plans purchased through the state health exchanges are also considered as OHI. In addition, veterans who purchase commercial insurance plans agree to cost-sharing responsibilities. Such cost-sharing obligations include copayments, deductibles, and coinsurance (e.g., 80/20 rule: 80% insurer responsibility/20% patient responsibility).
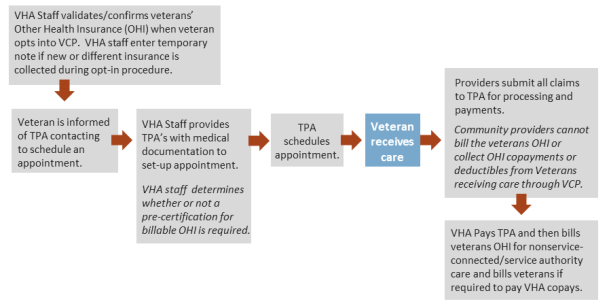
Due to various issues related to primary payment responsibility and veterans therefore experiencing adverse credit reporting to credit bureaus or debt collections by collections agencies, Congress enacted P.L. 115-26, which amended P.L. 113-146 and made VA the primary payer for veterans with OHI who seek care for nonservice-connected conditions through the VCP. This change went into effect on April 19, 2017. The VA would coordinate with a veteran's OHI and recover any costs, and bill the veteran for any copayments that the veteran would be responsible for similar to what they would have paid had they received care within a VA medical facility (see Figure 3). Community care providers or the TPAs are no longer required to collect copays, cost-shares, or deductibles from veterans with OHI. Medicare, Medicaid, or TRICARE are not considered OHI plans under the VCP.
Provider Payment Methodologies
Guidance on rates for the delivery of care is outlined in Table 4. As stated before, first, the Veterans Choice Program providers are to receive their reimbursements from the TPA. Then the VA is to reimburse the third-party administrator.55 Eligible VA community care providers who decide to participate under the PC3 network (rather than the Choice network) may incur reimbursement rates lower than those of Medicare.56 If these providers move to the Choice network, they may negotiate for a similar rate as contracted under the PC3 Network.
|
Episode of Care |
||
|
Service-Connected Condition |
Nonservice-Connected Condition |
|
|
Payment Responsibilities |
VA is solely responsible. |
|
|
||
|
Payment Rates |
Rates are not to exceed those in the "Medicare Fee Schedule," with exceptions in highly rural areas, Alaska, All-Payer Model Agreements, and when there are no available rates. |
|
|
Highly Rural Areasb |
|
|
|
Alaska |
|
|
|
All-Payer Model Agreements |
|
|
|
No Available Rates |
|
|
|
Authorized Care |
Health Net or TriWest, on behalf of the VA, will authorize services. |
|
|
The VA requires that all rendered services delivered to veterans receive prior authorizations. |
||
|
Medical services are delivered by an eligible entity or provider after a veteran chooses to receive care under the Veterans Choice Program. |
||
Source: 38 C.F.R. §17.1535.
a. On April 19, 2017, P.L. 115-26 made the VA the primary payer for medical care provided for any nonservice-connected condition. The VA was required to recover any costs from veterans' OHI plans. This removed the requirement that community providers and TPAs bill the veterans' OHI plans first.
b. A "highly rural area" is defined as a county having fewer than seven individuals residing per square mile.
Veterans and VA community care providers may call the Community Care Call Center57 to discuss billing issues. These issues range from the need to resolve a debt collection to inappropriately billed services.
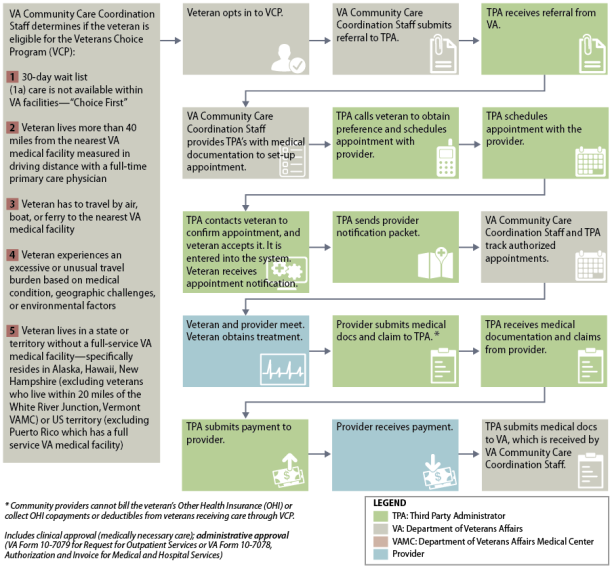
Appendix A. Veterans Choice Program (VCP) High-Level Work Flow
Appendix B. VA Information Pertaining to the End of the Contract with Health Net
 |
|
Source: Department of Veterans Affairs, Veterans Health Administration.
|
 |
|
Source: Department of Veterans Affairs, Veterans Health Administration.
|
 |
 |
|
Source: Department of Veterans Affairs, Veterans Health Administration. |
Author Contact Information
Acknowledgments
Amber Hope Wilhelm and Jose P. Ordoveza, CRS Visual Information Specialists, provided assistance with the figures in this report.
The author wishes to thank the staff of the Department of Veterans Affairs, Veterans Health Administration, Office of Congressional and Legislative Affairs, for their assistance in obtaining information.
Footnotes
| 1. |
Department of Veterans Affairs, Office of Inspector General, Review of Alleged Patient Deaths, Patient Wait Times, and Scheduling Practices at the Phoenix VA Health Care System, 14-02603-267, August 26, 2014. For a summary of wait-time issues at a VA medical facility, by state, see Department of Veterans Affairs Office of Inspector General, Administrative Summaries of Investigation Regarding Wait Times, http://www.va.gov/oig/publications/administrative-summaries-of-investigation.asp. Accessed on November 14, 2017. |
| 2. |
P.L. 113-146 as amended by P.L. 113-175, P.L. 113-235, P.L. 114-19, and P.L. 114-41. For a detailed provision-by-provision explanation of the act, see CRS Report R43704, Veterans Access, Choice, and Accountability Act of 2014 (H.R. 3230; P.L. 113-146). |
| 3. |
For a complete summary of the VA's standard medical benefits package, see CRS Report R42747, Health Care for Veterans: Answers to Frequently Asked Questions; and 38 C.F.R. §17.38. |
| 4. |
The 81 categories of medical services and procedures covered in the community under the VCP are acupuncture; allergy and immunology; audiology; biofeedback; cardiology catheterization; cardiology imaging; cardiology rehabilitation; cardiology stress test; cardiology tests, procedures, studies; chemotherapy; chiropractic; colonoscopy; dental; dermatology; dermatology tests, procedures, studies; endocrinology; endocrinology tests, procedures, studies; ear, nose, and throat; gastroenterology; gastroenterology tests, procedures, studies; genetic testing/counseling; gynecology; gynecology tests, procedures, studies; hematology/oncology; Hepatitis C; homemaker home health aid; hospice; hyperbaric therapy; infectious disease; interventional radiology; intravenous therapy (IV)/ infusion, clinic; lab and pathology; medicine; mental health; nephrology; neurology; neurology tests, procedures, studies; neuropsych testing; neurosurgery; newborn care; noninstitutional IV/infusion care; noninstitutional skilled home care; noninstitutional skilled nursing care; noninstitutional spinal cord care; nuclear medicine; nutrition/dietitian services; obstetrics; occupational therapy; ophthalmology; ophthalmology tests, procedures, studies; optometry; orthopedic; orthopedic tests, procedures, studies; pain management; physical therapy; plastic surgery; podiatry; primary care; pulmonary; pulmonary rehabilitation; pulmonary tests, procedures, studies; radiation therapy; radiology; radiology CT scan; radiology DEXA scan; radiology mammogram; radiology MRI/MRA; radiology PET scan; radiology ultrasound; rehabilitation medicine; respiratory therapy; rheumatology; sleep study/polysomnography; surgery general; thoracic surgery; urology; urology tests, procedures, studies; vascular; vascular tests, procedures, studies; veteran directed home and community based services; and wound care (Source: Department of Veterans Affairs, FY2018 Congressional Budget Submission, Medical Programs and Information Technology Programs, vol. 2 of 4, May 2017, pp. VHA-319-VHA- 320). |
| 5. |
Letter from Veterans Health Administration, Chief Business Office Purchased Care to Veteran, Eligible Choice 30-Day Wait Recipient, September 25, 2015. |
| 6. |
For general enrollment procedures, see CRS Report R42747, Health Care for Veterans: Answers to Frequently Asked Questions. |
| 7. |
Department of Veterans Affairs, "Expanded Access to Non-VA Care through the Veterans Choice Program," 80 Federal Register 74991-74996, December 1, 2015 (codified at 38 C.F.R.§17.1510). |
| 8. |
Department of Veterans Affairs, VA Care in the Community (Non-VA Purchased Care) and use of the Veterans Choice Program, Memorandum from Acting Principal Deputy Under Secretary for Health to Veterans Integrated Service Network (VISN) Directors, May 12, 2015, and amended on October 1, 2015. |
| 9. |
Local VA staff decides whether or not the burden is unusual or excessive and likely to exist "at least 30 days or more from the date of the determination." Staff are to document the decision on VA Form 119, Report of Contact, which includes the date of determination, expected duration of travel burden, and reason(s) behind the decision. Notification is to be sent in a letter by mail to the veteran. Department of Veterans Affairs, Veterans Health Administration, Veterans Choice Program - Unusual or Excessive Burden Determination, September 11, 2015. |
| 10. |
A local VA provider or the facility's Primary Care Patient Aligned Care Team (PACT) determines whether or not a veteran is facing an unusual or excessive travel burden due to a medical condition. The duration of the burden is also assessed. |
| 11. |
Veterans may appeal the decision of their local facility to the Board of Veterans Appeals (BVA). First, veterans would send a notice of disagreement to their facility. Then the facility is to generate a statement of case (SOC). Lastly, the facility is to process the appeal and forward it to the BVA for processing. Department of Veterans Affairs, Veterans Health Administration, Veterans Choice Program - Unusual or Excessive Burden Determination, September 11, 2015, p. 3. |
| 12. |
Department of Veterans Affairs, "Expanded Access to Non-VA through the Veterans Choice Program," 79 Federal Register 65577, November 5, 2014 (codified at 38 C.F.R. §17.1515). |
| 13. |
38 C.F.R. §17.1515. |
| 14. |
38 C.F.R. §17.1530. |
| 15. |
38 C.F.R. §17.1530. |
| 16. |
Secretary Robert A. McDonald, An Open Letter to America's Veterans, Department of Veterans Affairs, Veterans Health Administration, 2014, http://www.va.gov/opa/choiceact/documents/Open-Letter-to-Veterans.pdf. Accessed on December 29, 2017. |
| 17. |
Department of Veterans Affairs, Veterans Choice Program, Leadership Toolkit for VA Facilities, p. 16. |
| 18. |
Health Net Federal Services, Overview of Health Net Federal Services' VA Programs, https://www.hnfs.com/content/hnfs/home/company/company-information/va.html. Accessed on December 29, 2017. |
| 19. |
TriWest Healthcare Alliance, http://www.triwest.com/en/veteran-services/veterans-choice-program-vcp/. Accessed on January 2, 2018. |
| 20. |
The Patient-Centered Community Care (PC3) initiative evolved from the Project on Healthcare Effectiveness through Resource Optimization (Project HERO) pilot program. Under the PC3 program, VA provides contracted inpatient and outpatient specialty care and mental health care to eligible veterans when VA medical facilities cannot provide services such as when there is a lack of medical specialists, or long wait times, or there is an extraordinary long distance from the veteran's residence. |
| 21. |
Veterans Health Administration, Choice Champion Call, November 10, 2015, p. 31. |
| 22. |
Department of Veterans Affairs, "Contract with Health Net Federal Services to End," Fact Sheet, March 2018. |
| 23. |
Senate Committee on Veterans' Affairs, "Tester, Crapo Hold Health Net Accountable For 'Poor Performance," press release, March 13, 2013, https://www.veterans.senate.gov/newsroom/minority-news/tester-crapo-hold-health-net-accountable-for-poor-performance, and https://www.veterans.senate.gov/download/shulkin-re-health-net. Accessed April 18, 2018. |
| 24. |
Major portions of this section are adapted from, Department of Veterans Affairs, Veterans Health Administration, How to become a Veterans Choice Program and/or Patient-Centered Community Care Provider, VA Community Care Fact Sheet for Interested Providers, May 24, 2017, p. 2. https://www.va.gov/opa/choiceact/documents/How_to_Become_VA_Provider_05242017_508.pdf. Details on how providers could participate in VCP are available at https://www.va.gov/opa/choiceact/for_providers.asp. Accessed on January 2, 2018. |
| 25. |
Under the PC3 program, VA provides contracted inpatient and outpatient specialty care and mental health care to eligible veterans when VA medical facilities cannot provide services such as when there is a lack of medical specialists, or long wait times, or there is an extraordinary long distance from the veteran's residence. |
| 26. |
TriWest may be contacted by phone (1-866-284-3743) or email ([email address scrubbed]). For additional information about TriWest, see https://www.triwest.com/provider. Accessed on January 2, 2018. |
| 27. |
The Centers for Medicare and Medicaid Services manages the Medicare Exclusion Database (MED) which contains a list of excluded providers and their sanctions and reinstatement files. For additional information about the MED, see https://www.cms.gov/Research-Statistics-Data-and-Systems/Computer-Data-and-Systems/MED/Overview-MED.html. Accessed on January 2, 2018. |
| 28. |
To determine if a provider or entity is required to meet the Conditions of Participations (CoPs) and Conditions for Coverage (CfCs), see https://www.cms.gov/Regulations-and-Guidance/Legislation/CFCsAndCoPs/index.html. Accessed on January 2, 2018. |
| 29. |
Veterans Choice Program (VCP) Provider Agreements may be authorized between local VA Medical Centers (VAMCs) and out-of-network VA community care providers only after TriWest is unable to process a veteran's authorization request and/or schedule an appointment, within a timely manner, for the veteran. |
| 30. |
Major portions of this section are adapted from, Department of Veterans Affairs, Veterans Health Administration, VHA Chief Business Office, Veterans Choice Program, Unusual or Excessive Burden Determination (Other Factors) Process, December 2015. |
| 31. |
Generally, a veteran who becomes eligible under the VCP through the "30-day wait list" or "40 miles or more distance" pathway may not have to go through the entire VA community care consult/referral process. |
| 32. |
The Computerized Patient Record System (CPRS) is the electronic system VA providers use to input consults/referrals for VA community care. Once entered, the VA community care consult/referral is to alert a clinical reviewer who is to examine the veteran's medical need and confirm that the requested services are not available at a local VA health care facility. |
| 33. |
Special authority conditions include those that are eligible for service-connection under Priority Group 6 (combat veterans, ionization radiation, Agent Orange exposure, Southwest Asia service, veterans stationed at Camp Lejeune between August 1, 1953 to December 31, 1987, and Project 112/ SHAD), military sexual trauma, nasopharyngeal radium irradiation, etc. |
| 34. |
"R-UR, under the auspices of the CBO, is the systematic evaluation and analytical review of clinical information in order to maximize reimbursement from third-party payers. In 2003, guidance was established standardizing the clinical review functions with third-party reimbursement responsibilities at VA medical facilities. R-UR in this context operates to promote improvements in patient care and to maximize the potential for the recovery of funds due VA for the provision of health care services to Veterans, dependents, and others using the VA health care system." For more information, see Department of Veterans Affairs, Veterans Health Administration, Utilization Management Program, VHA Directive 1117, Washington, DC, July 9, 2014, p. 8, http://www.va.gov/vhapublications/ViewPublication.asp?pub_ID=3018. Accessed on January 2, 2018. |
| 35. |
Major portions of this section are adopted from Department of Veterans Affairs, Veterans Health Administration, VHA Chief Business Office, Veterans Choice Program, Unusual or Excessive Burden Determination (Other Factors) Process, December 2015. Also see, Department of Veterans Affairs, Veterans Health Administration, Veterans Choice Program (VCP), Fact Sheet: Details on the Unusual or Excessive Burden Eligibility Criteria, May 27, 2017, https://www.va.gov/COMMUNITYCARE/docs/pubfiles/factsheets/VHA-FS_VCP-Eligibility.pdf. Accessed March 28, 2018. |
| 36. |
An attendant for clinical services is a person who provides essential aid and/or physical assistance to the veteran so that the veteran can travel to a VA medical facility to have hospital care or medical services rendered. 38 C.F.R. §17.1510(b)(4)(ii)(A)-(C). |
| 37. |
VA community care providers may call the Operation Center for Choice at [phone number scrubbed] to request prior authorization from TriWest prior to delivering medical services to veterans. Failure to obtain preauthorization prior to rendering health services may result in uncompensated services. |
| 38. |
38 C.F.R. §17.1505. |
| 39. |
Ibid. |
| 40. |
Department of Veterans Affairs, "Expanded Access to Non-VA Care Through the Veterans Choice Program," 80 Federal Register 66424, October 29, 2015. |
| 41. |
Veterans Health Administration, Ten Things to Know About the Choice Program, 2015, http://www.va.gov/HEALTH/newsfeatures/2015/July/10-Things-to-Know-About-Choice-Program.asp. Accessed on January 2, 2018. |
| 42. |
Department of Veterans Affairs, Veterans Health Administration, Prescription Reimbursement Associated with VACC Delivered under the Choice Program, VA Care in the Community (VACC) Program Reference Sheet, October 27, 2015. Department of Veterans Affairs, "Expanded Access to Non-VA Care Through the Veterans Choice Program," 79 Federal Register 65572, November 5, 2014. |
| 43. |
Department of Veterans Affairs, VA Office of Inspector General, Veterans Health Administration, Audit of Timeliness and Accuracy of Choice Payments Processed Through the Fee Basis Claims System, 15-03036-47, December 21, 2017, p. 6. |
| 44. |
Department of Veterans, VA Office of Inspector General , Bulk Payments Made under Patient-Centered Community Care/Veterans Choice Program Contracts, Report #17-02713-231, September 6, 2018, p. 5. |
| 45. |
Department of Veterans Affairs, Veterans Health Administration, Working with the Veterans Health Administration: A Guide for Providers, October 2014, p. 3, https://www.va.gov/COMMUNITYCARE/docs/pubfiles/programguides/NVC_Providers_Guide.pdf. Accessed on January 2, 2018. |
| 46. |
The standard billing forms for reimbursement include the UB-04 CMS-1450 or CMS-1500. |
| 47. |
38 C.F.R. §17.124. |
| 48. |
VA Form 10-583, Claim for Payment of Cost of Unauthorized Medical Services, at http://www.va.gov/vaforms/form_detail.asp?FormNo=583. Accessed on January 2, 2018. |
| 49. |
An amount paid, by an enrollee or by an employer or a combination of both parties, to an insurer for a beneficiary to enroll in a health insurance plan. |
| 50. |
An amount a beneficiary must pay out of pocket before the health insurance plan begins paying for services. |
| 51. |
A specified percentage a beneficiary pays out of pocket to a provider after meeting any deductible requirements. |
| 52. |
Only veterans in Priority Group 1 (those who have been rated 50% or more service-connected) and veterans who are deemed catastrophically disabled by a VA provider are never charged a copayment, even for treatment of a nonservice-connected condition. For more information, see Department of Veterans Affairs, "Criteria for a Catastrophically Disabled Determination for Purposes of Enrollment," 78 Federal Register 72576-72579, December 3, 2013. |
| 53. |
The VA categorizes veterans into eight Priority Groups, based on factors such as service-connected disabilities and income (among others). For a detailed summary of eight Priority Groups, see CRS Report R42747, Health Care for Veterans: Answers to Frequently Asked Questions. |
| 54. |
38 C.F.R. §§17.108, 17.110, 17.111. |
| 55. |
Department of Veterans Affairs, VA Office of Inspector General, Veterans Health Administration, Audit of Timeliness and Accuracy of Choice Payments Processed Through the Fee Basis Claims System, 15-03036-47, December 21, 2017, p. 6. |
| 56. |
Department of Veterans Affairs, "Expanded Access to Non-VA Care Through the Veterans Choice Program," 80 Federal Register 66425, October 29, 2015. |
| 57. |
Veterans may call the Community Call Center at 1-877-881-7618 from 9 am to 5 pm EST (https://www.va.gov/HEALTHBENEFITS/cost/disputes.asp). Accessed on January 2, 2018. |