The Opioid Epidemic and the Labor Force
Some Members have expressed strong concerns about the societal costs of the opioid epidemic, including its potential to adversely affect the U.S. economy. Efforts to quantify the annual economic costs of opioid abuse and dependence return estimates in the tens of billions, of which workforce losses—decreased productivity, missed days of work, and premature death—account for a substantial share. Opioid abuse could further generate labor force costs—directly or indirectly—if it affects labor force participation decisions and unemployment. A small body of research has explored and identified correlations between opioid abuse and these indicators, but it remains unclear whether the opioid epidemic is a driver or an outcome of recent workforce trends, or an indicator of other underlying factors.
Opioids and Non-Participation in the Labor Force
The labor force comprises employed workers and non-employed workers who are actively seeking and available for work (i.e., the unemployed); persons who are neither working nor searching for work are said to be out of the labor force. Policymakers view the labor force participation rate (LFPR) as an important economic indicator because the labor force is a key determinant of economic output. For this reason, the decades-long decline in the LFPR of prime-age (i.e., ages 25-54 years) men and more recent drops in prime-age women's LFPR have raised questions about the country's ability to reach its full economic potential. Labor force participation decisions are complex, and research identifies several factors as potential contributors to these LFPR patterns including fewer jobs for less-educated workers, poor health and disability, employment barriers for a growing population with criminal records, and increased disincentives to work; Krause and Sawhill provide a recent review of this research.
While generally not viewed as a primary driver of recent workforce trends, some have pointed to the opioid epidemic as one contributor to recent declines in LFPRs. For example, during the question-and-answer portion of her July 2017 testimony to the Senate Committee on Banking, Housing, and Urban Affairs, Federal Reserve chairwoman, Janet Yellen cited the epidemic as a potential factor (among others) influencing LFPRs among prime-age men, referencing recent research on the increase in "deaths of despair," including from drug overdose, among some populations.
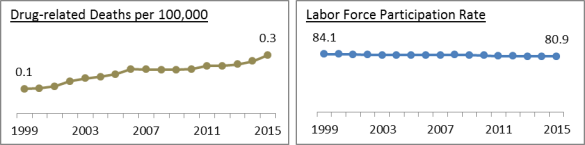
Data on drug-related deaths and emergency department visits, and opioid prescriptions appear to support this viewpoint. Figure 1 shows that the rate of drug related deaths (of which opioids are the main cause) rose markedly for prime-age persons over the 1999-2015 period, as the LFPR for this group declined by more than 3 percentage points. Work by Hollingsworth et al. shows a 39.5% increase in emergency department visits involving opioids between 2006 and 2014, with prime-age persons representing most visits (link requires paid subscription). Preliminary estimates by Krueger provide the most rigorous exploration of the relationship between opioid prescriptions and labor force participation. Krueger found that prime-age men's LFPR was lower and fell more over a 15-year period in counties with high opioid prescriptions per capita; he found similar results for the decline in prime-age women's LFPR.
|
Figure 1. Drug-related Deaths (per 100,000) and Prime-Age Labor Force Participation Rate, 1999-2015 |
 |
|
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, Multiple Cause of Death 1999-2015. Bureau of Labor Statistics, Current Population Survey Program. Notes: Prime-age persons are those ages 25-54 years. |
Opioids and Worker Outcomes
Research has also explored connections between opioid abuse and outcomes for unemployed and employed workers. Hollingsworth et al. find that "opioid deaths and emergency department visits are predicted to rise when county unemployment rates temporarily increase" and find similar results for state-level analyses (link requires paid subscription). This correlation between drug abuse and unemployment aligns with recent reporting on employers' struggle to find job applicants who can pass a drug test that screens for opioids and other drugs.
Public health studies identify additional opioid-related costs incurred by employed workers, resulting from diminished job performance, additional days of missed work (including for incarceration), and premature death. Florence et al. estimate such lost productivity costs for 2013 to be $20 billion ($16 billion from reduced productive time and increased disability, and $4 billion for production lost for incarcerated individuals) (link requires paid subscription). Earlier studies produce similar estimates, for example Hansen et al. (link requires paid subscription) and Birnbaum et al.
Opioids: Cause or Consequence of Adverse Labor Market Outcomes?
It is yet unclear whether the opioid epidemic is a driver of low labor force participation and other workforce trends or an outcome of a lack of job opportunities. It is possible that the increased supply of opioids has expanded or intensified drug abuse such that opioid users interest in or suitability for work has declined, i.e., opioids cause detachment from the work. Another possibility—related to work by Case and Deaton and Pierce and Schott—is that declining job opportunities, particularly for less-skilled workers, has led to increased drug use and other health-deteriorating behavior (i.e., opioid use is a consequence of economic conditions). These scenarios are not mutually exclusive; opioids may both contribute to and result from weak labor market outcomes.
A more complex relationship may exist as well. Krueger's research, for example, shows increased reports of pain and disability among labor market nonparticipants. This raises the possibility that injury or disability is a causal factor for nonparticipation, and increased opioid use is an indicator of this trend. Even if opioid use has a limited role in causing labor market separations, increased reliance on pain medication may have made it more difficult for nonparticipants to return to work. Case and Deaton observe that while opioids may not be the "fundamental factor" of rising mortality and morbidity among white middle-age workers, "the prescription of opioids for chronic pain added fuel to the flames, making the epidemic much worse than it otherwise would have been."
Additional information on the studies cited herein is available from CRS.